2nd Place Emage Winner: Fibrosing Mediastinitis
Olena Kostyuk, MD
Amy Sparkman, MD
Jamie Laughy, MD
Oklahoma Children’s Hospital
Case Description
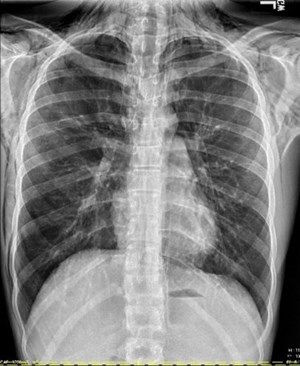
A 14-year-old boy presented to the emergency department after a mediastinal mass was identified on a chest x-ray by his primary care physician. The patient had a chronic cough for several years and had recently lost approximately 50 lbs over 2-3 months. On initial presentation, he was hemodynamically stable with normal vital signs and an unremarkable physical examination.
Laboratory studies upon admission were normal except for an elevated white blood cell (WBC) count of 15.6. Uric acid and lactate dehydrogenase (LDH) levels were normal. Blood flow cytometry was negative for leukemia or lymphoma.
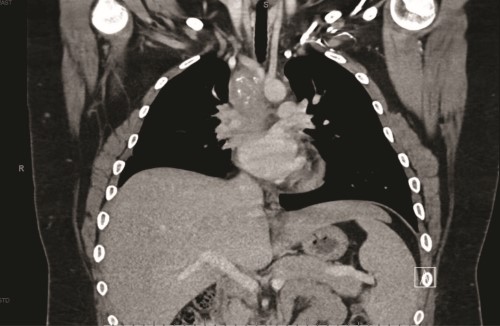
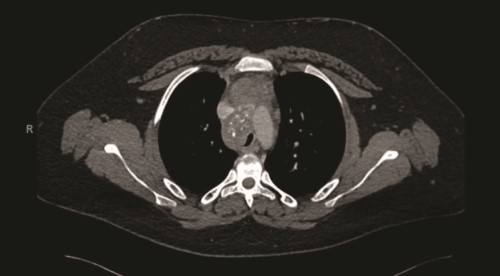
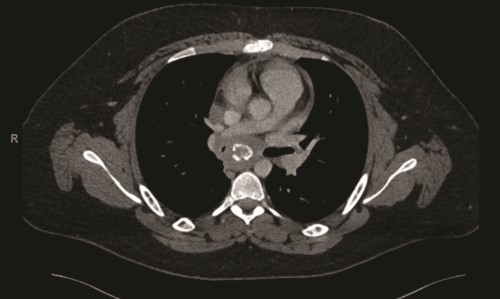
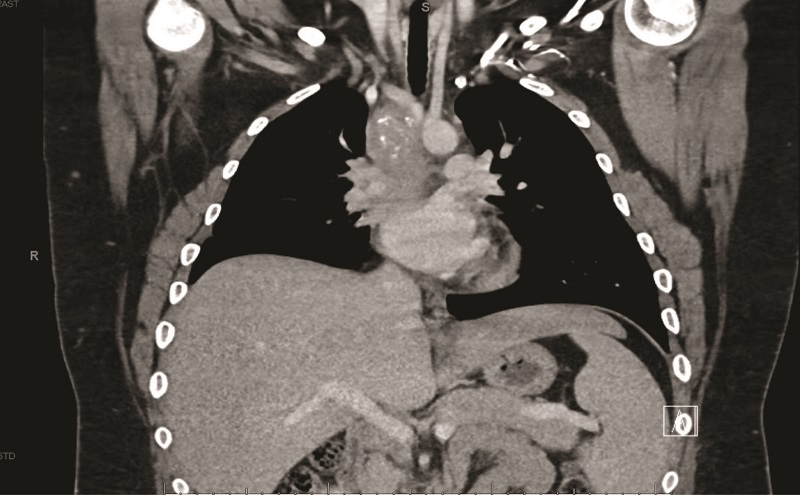
A contrast-enhanced computed tomography (CT) scan of the chest revealed a confluent calcified tissue density mass surrounding the subcarinal, right peritracheal, and anterior mediastinal region, causing significant extrinsic compression of the mid and distal trachea and right main stem bronchus, narrowing of the pulmonary artery, and partial encasement of the azygos vein.
Further workup included negative results for histoplasma serum and urine antigens, but the histoplasma antibody M band was detected. Human immunodeficiency virus (HIV) and tuberculosis testing were negative. A pathology report from a biopsy of the mediastinal mass showed no evidence of malignancy, alveolar macrophages with chronic inflammation and necrotic debris.
Imaging and laboratory findings were consistent with fibrosing mediastinitis likely due to previous Histoplasma infection. The patient was discharged home on itraconazole with a plan for surgical excision of the mediastinal mass.
Discussion
Fibrosing mediastinitis (FM) is a rare fibroinflammatory disorder characterized by dense fibrous tissue proliferation in the mediastinum, potentially encasing bronchovascular structures. In the United States, most cases are linked to previous infection with Histoplasma capsulatum, but other infectious, autoimmune, and malignant conditions must be ruled out.
Most patients remain asymptomatic, with diagnosis often made incidentally on cross-sectional radiography. However, some patients develop significant compression of mediastinal structures.
Contrast-enhanced CT is the most effective diagnostic tool, revealing a variably enhanced soft tissue mass with calcification, and possible encasement or obstruction of airway and vascular structures.
FM should be considered a differential diagnosis in patients with mediastinal vascular compression and related imaging findings.
Management depends on disease severity and may include medical treatment with anti-inflammatory agents, antifungal therapy, and surgical intervention.
Images
CT of the chest with contrast showed a partially calcified soft tissue mass in the right paratracheal region, extending around the inferior trachea, carina, and proximal mainstem bronchi. The mass measured approximately 8.1 x 6.2 x 7.6 cm.