Popliteal Sciatic Nerve Block
Leonard V. Bunting, MD, FACEP
I. Introduction and Indications
- The ability to block the sciatic nerve is a powerful tool in the emergency setting.
- Accessing the sciatic nerve proximally is challenging due to its deep lie but the nerve becomes superficial as it approaches the popliteal fossa allowing for relatively easy blockade.
- Blocking the nerve near the popliteal fossa still covers part of the knee and distal leg, making it excellent for injuries to the lower leg, especially the ankle.
- The popliteal block does not cover the medial leg; therefore, consider also blocking the femoral or saphenous nerve for injuries involving the whole distal lower extremity, such as bimalleolar fractures.
Anatomy
- Sciatic nerve originates from the lumbar and sacral plexus (L4 – S3) and travels deeply in the posterior thigh.
- Proximal to the popliteal fossa, the sciatic nerve lies more superficial, between the long head of the biceps femoris laterally and the semimembranous muscles medially.
- Approximately 6 cm above the popliteal crease, the nerve bifurcates into the common peroneal and tibial nerves. These nerves continue into the popliteal fossa where they lie superficial and lateral to the popliteal vessels.
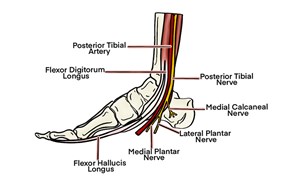
- The tibial nerve continues down the back of the leg to wrap around the posterior medial malleolus. It provides innervation to the majority of the posterior lower extremity, knee joint and plantar surface of the foot.
- The common peroneal nerve passes posterior to the head of the fibula and then winds anteriorly, where it divides into deep and superficial branches. The common peroneal nerve provides sensory innervation to the dorsal lateral foot and ankle, and posterolateral portion of the distal lower extremity via its branches.
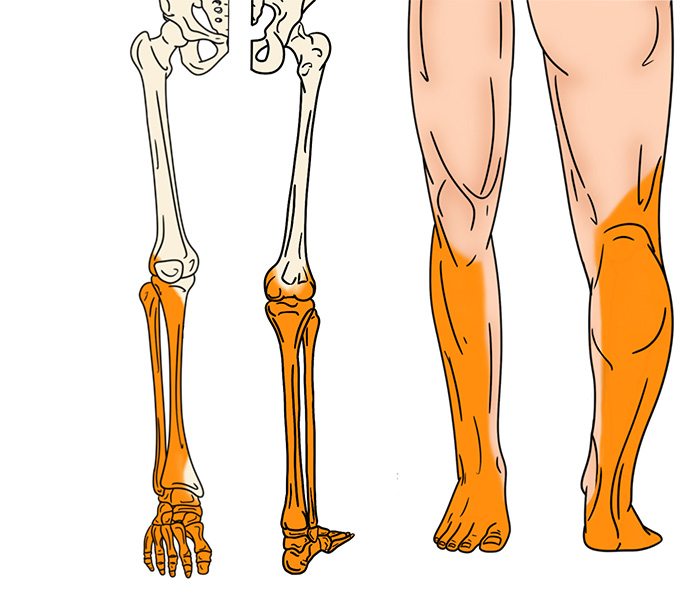
Illustration 1. Distribution of anesthesia of popliteal sciatic block
Indications
- Management of painful conditions below the knee (burns, fractures, dislocations, infections)
- Procedural anesthesia for reduction of the ankle or foot and manipulation of fractures of the tibia, fibula or foot
Contraindications
- General block contraindications
- Injuries at risk of compartment syndrome, especially tibia fractures
- Injuries isolated to the medial leg (covered by saphenous nerve)
II. Equipment
- Skin prep and sterile probe cover
- 5-12 MHz linear array probe
- 27-gauge needle and syringe of 3-5 cc of 1% lidocaine with epi for skin anesthesia
- 3.5-inch, 20-22-gauge spinal needle
- 30cc syringe with anesthetic of choice
III. Setup and Patient Positioning
- General procedure setup
- Ultrasound machine is usually placed on the opposite side of the bed from the block site.
- Ideal patient position is prone. Decubitus position with target leg up is possible, but probe and needle handling is more challenging.
- Support leg as needed during positioning.
IV. Pre-scan and Sonographic Anatomy
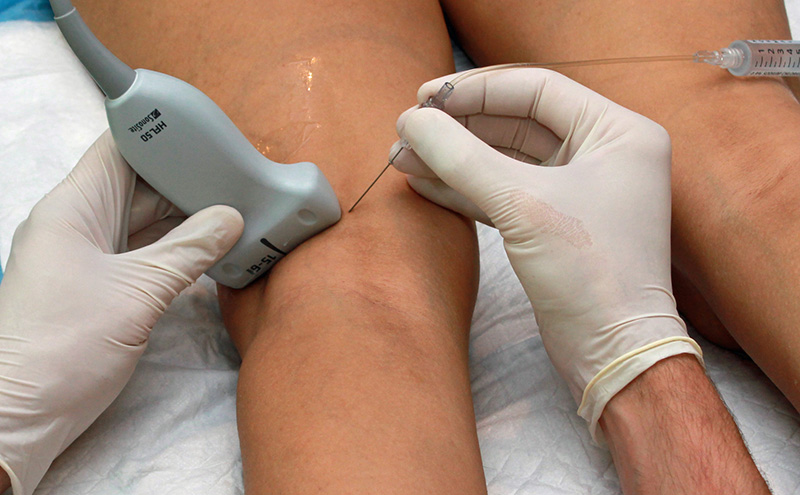
- Place a high-frequency linear array probe in the popliteal fossa. (Figure 1)
- Orient probe indicator to the operator’s left.
- Set depth to 4-6 cm, depending on patient’s body habitus.
- Identify the pulsatile popliteal artery and corresponding vein superficial and medial to the femur.
- Superficial to the popliteal vessels identify the tibial nerve.
- Always adjust the angle of insonation (tilt of the probe relative to the skin) to improve the echogenicity of the nerve.
- If visualization is still challenging, the patient can plantar flex the ankle to elevate the peroneal nerve and dorsiflex the ankle to elevate the tibial nerve. This is commonly referred to as the “seesaw” sign.
Video 1. Pre-scan of the popliteal block
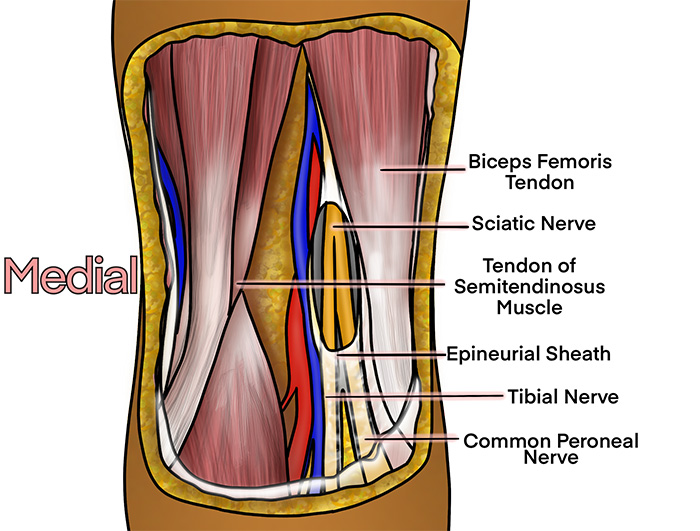
Illustration 2. Course of the popliteal sciatic nerve
Video 2. Seesaw technique of nerve localization
- Trace the tibial nerve proximally until it joins the common peroneal nerve to become the sciatic nerve. Again, if visualization of the nerves is difficult, the probe is tilted to find the ideal angle of insonation with the nerve.
- If the sciatic nerve is well visualized and not too deep, this will be the target for the nerve block. If the sciatic nerve is not visualized, consider the tibial and common peroneal nerves as the targets.
V. Technique
- In-plane approach is preferred from whichever side is most comfortable.
- Probe indicator oriented to operator’s left.
- Center the target nerve(s) on the image.
- Sciatic nerve is the target if well visualized and accessible.
- If blocking after the bifurcation, inject the nerve furthest from the needle first to prevent anesthetic injection from pushing one nerve farther away.
- Insert the block needle 1 cm at ~45 degrees to the skin surface.
- Visualize the needle and ensure the needle is always in view.
- Slowly advance the needle towards the deep, proximal border of the nerve.
- Once movement of the needle causes movement on the nerve, injection may begin.
- Follow injection precautions.
- Initially inject 0.5cc.
- Appropriate needle placement is confirmed by anesthetic flowing around the entire nerve.
- Readjustment of the needle position may be necessary to achieve adequate distribution of anesthesia.
- Always perform aspiration and incremental injection to avoid systemic distribution of the anesthetic.
- Typical block volumes are 15–30cc.
- Full block onset may take up to 15–20 minutes, particularly if a long-acting anesthetic was used.
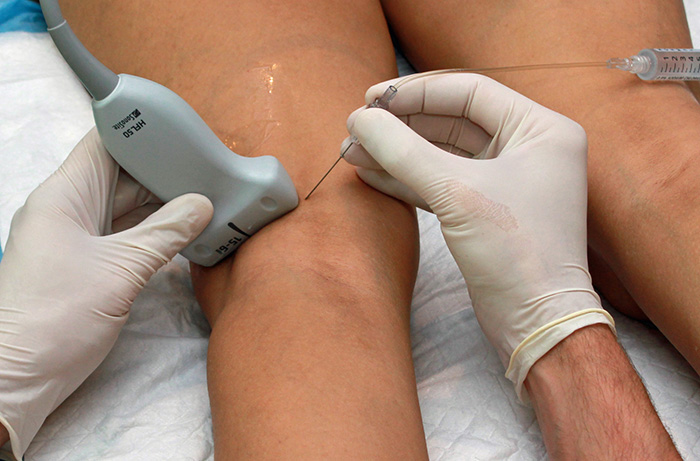
Figure 1. Hands in the popliteal fossa
Video 3. Popliteal block after bifurcation
VI. Pearls and Pitfalls
- Ensure that all nerves are blocked. The tibial nerve is large and can be easily mistaken for the sciatic nerve leading to no anesthesia in the region of the peroneal nerves.
- Maintain a shallow needle angle. It will greatly enhance needle visualization.
- If also blocking the femoral or saphenous nerves, monitor the combined doses to avoid toxicity.
- In this region, the nerve’s appearance is affected by the angle of the probe, which is called anisotropy. If the nerve does not appear hyperechoic to surrounding structures, change your angle of insonation by tilting the probe.
- Avoid injecting too much local anesthetic into the surrounding muscle. It will make the muscle hyperechoic and decrease contrast from the nerve.
VII. Resources
- Sinha A, Chan VW. Ultrasound imaging for popliteal sciatic nerve block. Reg Anesth Pain Med. 2004;29:130-4.
- Gray AT, Huczko EL, Schafhalter-Zoppoth I. Lateral popliteal nerve block with ultrasound guidance. Reg Anesth Pain Med. 2004;29:507-9.
- Sites BD, Gallagher JD, Tomek I, Cheung Y, Beach ML. The use of magnetic resonance imaging to evaluate the accuracy of a handheld ultrasound machine in locating the sciatic nerve in the popliteal fossa. Reg Anesth Pain Med. 2004;29:413-6.
- Schafthalter-Zoppoth I. The “see-saw” sign: improved sonographic identification of the sciatic nerve. Anesthesiology. 2004;101:808-9.