Radial Nerve Block
Andrew Butki, DO
Leonard V. Bunting, MD, FACEP
I. Overview/Indications
- Ultrasound guided regional anesthesia is being performed by emergency physicians at most academic emergency departments.1
- Nerve blocks of the forearm are safe and provide an effective alternative to sedation and to opioid analgesics for pain management in the emergency department, with high levels of satisfaction among both patients and physicians.2-4
- Forearm blocks should be considered as an alternative to digital blocks; the duration can be much longer, and it doesn’t require the pain, pressure and distortion of injecting into the finger’s small volume.
- There is overlap of the hand’s sensory territory.
- The radial nerve provides innervation to the dorsum of the hand but provides exclusive innervation to only a small portion of this area.5
- Consider providing blockade of ulnar nerve +/- median nerve +/- radial nerve for most injuries.
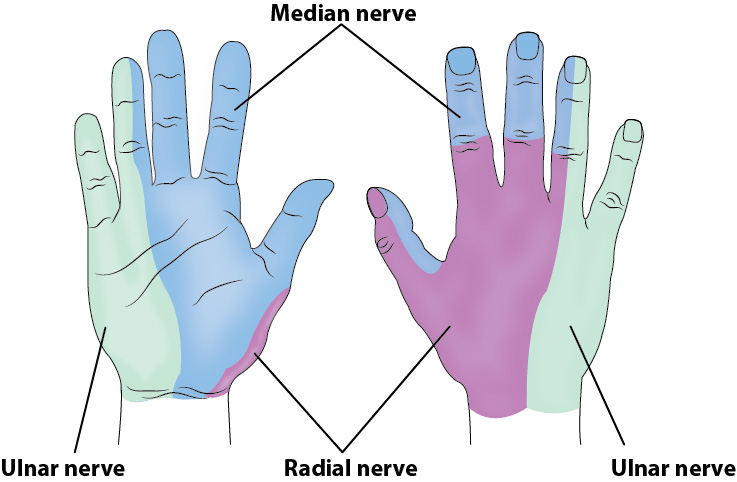
Illustration 1. Distribution of anesthesia
Indications
- Dorsal hand lacerations, burns, abscesses, foreign bodies, or any soft tissue injury to the hand and wrist.
- Forearm nerve blocks in general are not as useful for fractures of the wrist.
- These require a more proximal block above the elbow.
- Forearm blocks miss the posterior interosseous nerve. The radial nerve bifurcates above the elbow. When blocking the radial nerve at the forearm, only the superficial branch is blocked. In order to block both the deep and superficial branches, a proximal approach is required.6
- Generally, the innervation of the bones (osteotomes) follow their own pattern that does not coincide with the innervation of the skin or more superficial structures (dermatomes).7
Contraindications
II. Equipment
- Probe selection: 6-12 MHz linear transducer
- Sterile transparent film dressing (eg, Tegaderm™) or sterile probe cover
- 7-10ml of anesthetic
- 27-gauge needle for skin wheal with syringe of 2-3 ml of lidocaine with epinephrine
- 20-22-gauge needle, 1.5 inch or longer (Needle choices) depending on body habitus
III. Setup and Patient Positioning
- General procedure setup
- Patient sitting upright
- Forearm supine and abducted, externally rotated to provider and patient’s comfort
IV. Pre-scan/Sonographic Anatomy
Anatomy
- At the elbow, the radial nerve passes anterior to the lateral epicondyle. Upon entering the cubital fossa, it immediately splits into a deep and superficial branch. The deep branch provides motor innervation and the superficial branch supplies sensory innervation to the dorsum of the hand.
- In the proximal forearm, the radial nerve runs deep to the brachioradialis muscle, giving off several articular branches.8 For this reason, block the radial nerve as proximal in the forearm as possible to maximize distribution of anesthesia.
- In the mid-forearm, the radial nerve is tightly associated with the lateral side of the radial artery and travels in the same fascial plane.
- In the distal forearm, the radial nerve separates into posterior sensory branches and rolls laterally around the radius.
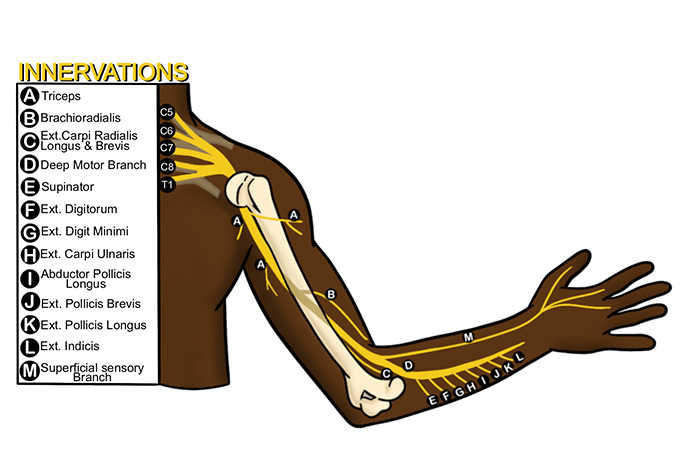
Illustration 2. Course of the radial nerve
Pre-scan
- Place the probe transversely on the volar surface of the forearm.
- Slide the probe laterally to identify the pulsatile radial artery.
- Directly lateral to the radial artery should be a hyperechoic structure representing the radial nerve.
- The nerve can be oval or triangular.
- The radial nerve sits in the same echogenic fascial plane as the artery.
- If not immediately seen, rapidly slide up and down the radial artery from the mid-forearm to identify the nerve associating with the artery.
- Moving proximally, it will separate from the artery and stay on the lateral forearm as the radial artery courses medial to the brachial artery.
- Moving distally, it will separate, flatten and roll laterally around the radius to form the cutaneous branches.
Video 1. Radial nerve pre-scan
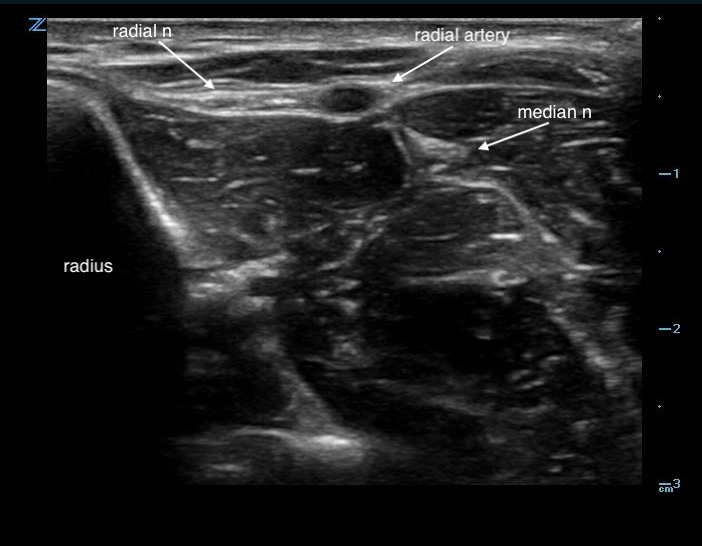
Figure 1. Sonographic appearance of the radial nerve in the mid-forearm
V. Procedure Technique
- Use standard sterile skin preparation.
- Cover probe using sterile transparent film dressing (ie, Tegaderm™) or sterile probe cover.
- Flush all needles of air, as air obscures ultrasound imaging.
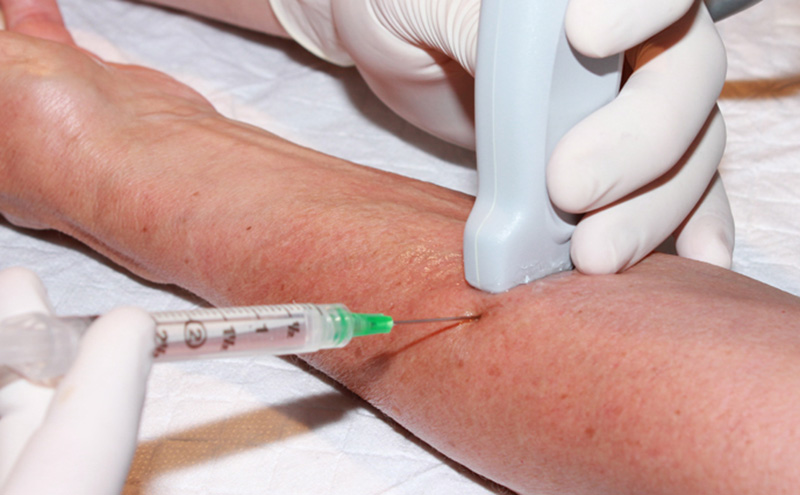
- In-plane approach is recommended (Needle orientation) from a direction that avoids the radial artery.
- Create skin wheal using 25-30-gauge needle.
- Insert block needle 5 mm at the short side of the probe with bevel pointing upwards.
- Visualize the needle.
- Aim for bottom of nerve.
- This helps avoid injuring nerve.
- Injected fluid will naturally push superficially, following path of least resistance.
- Advance until you achieve “mechanical coupling”, where the blunt portion of your needle is in direct contact with the nerve and movement of the needle causes movement of the nerve.
- Inject a test of 0.5 mL of anesthetic to confirm location.
- Follow general block contraindications.
- If you are appropriately within the perineural space, your anesthetic will envelop the nerve and seem to push the nerve away from the needle.
- If you are not close enough, your anesthetic will create a bolus of anesthetic directed away from the nerve.
- Once appropriate placement is confirmed, inject the remainder of the anesthetic until you have enveloped the nerve on at least 3 sides, preferably all sides.
- It is imperative that anesthetic is seen between the radial nerve and artery.
- Typical volumes are 5-10 ml.
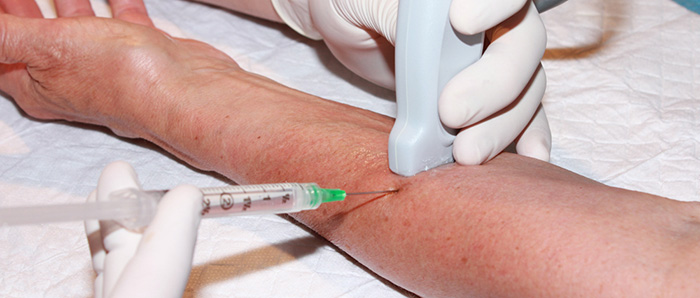
Figure 2. Hand placement for in-plane radial nerve block
Video 2. In-plane radial nerve block
VI. Post-procedure Care
Consider marking on skin with skin pen the time and date of block performed.
VII. Pearls and Pitfalls
- An out-of-plane approach can be used as well and may assist in depositing anesthetic between the nerve and artery.
- Inadequate anesthesia may result from blockade of the radial nerve alone. Consider blocking two or all three forearm nerves, as there is a lot of overlap in the regions covered by each nerve.
- All nerves display anisotropy (ie the nerve is significantly more visible when your probe is perfectly perpendicular to the nerve). Fanning your probe as you scan up and down the forearm can improve visualization of the median nerve.
- Too short or too thin a needle will make needle progression difficult, especially in a patient with very large or muscular forearms.
- The most painful part of the procedure is the initial skin puncture, which is why a small local anesthetic skin wheal is recommended.
- The majority of the needle path is through musculature, which is usually well tolerated by patients (skeletal muscle fibers themselves do not receive direct innervation by free Type C nerve endings).9
- More advanced users can consider performing the block with smaller needles (eg, 25 gauge).
- Usually only 5-7 mL of anesthetic is required, and so systemic toxicity is unlikely. However, if multiple blocks are performed (median, ulnar, and radial nerve) with larger volumes it is possible to approach or even cross the threshold for toxicity.
VIII. References
- Richard A, Jeffrey K, Arun N, Srikar A. Ultrasound-guided nerve blocks in emergency medicine practice. J Ultrasound Med. 2016;35(4):731-6.
- Nejati A, Teymourian H, Behrooz L, Mohseni G. Pain management via ultrasound-guided nerve block in emergency department; a case series study. Emerg (Tehran). 2017: 5(1):e12.
- Bhoi S, Rodha M, Ramchandani R, Sinha T, Bhasin A, Galwankar S. Feasibility and safety of ultrasound-guided nerve block for management of limb injuries by emergency care physicians. J Emerg Trauma Shock. 2012;5(1):28-32.
- Liebmann O, Price D, Mills C, Gardner R, Wang R, Wilson S, et al. Feasibility of forearm ultrasonography-guided nerve blocks of the radial, ulnar, and median nerves for hand procedures in the emergency department. Ann Emerg Med. 2006;48:558-62.
- Mackinnon S, Fox I, et al. Peripheral nerve surgery: A resource for surgeons. Washington University School of Medicine, 2010.
- Frenkel O, Herring AA, Fischer J, Carnell J, Nagdev A. Supracondylar radial nerve block for treatment of distal radius fractures in the emergency department. J Emerg Med. 2011;41(4):386-8.
- Carrera A, Lopez A, Sala-Blanch X, et al. Functional Regional Anesthesia Anatomy. New York School of Regional Anesthesia.
- Moore K, Dalley, A. Clinically Oriented Anatomy, 5th Lippincott Williams and Wilkins, 2006.
- Mense S, Gerwin R. Muscle Pain: Understanding the Mechanisms. Springer 2010. ISBN: 978-3-540-85020-5.