Tibial Nerve Block
Leonard V. Bunting, MD, FACEP
I. Introduction and Indications
- The ability of the emergency physician to block the tibial nerve is crucial.
- Injuries and procedures in the sole of the foot are common in the ED, and cutaneous injection into this region can be extremely painful.
- Blind blockade has a reported success rate as low at 22%. Ultrasound dramatically improves the ease and efficacy of this procedure.1
Anatomy
- The tibial nerve is a distal branch of the sciatic nerve.
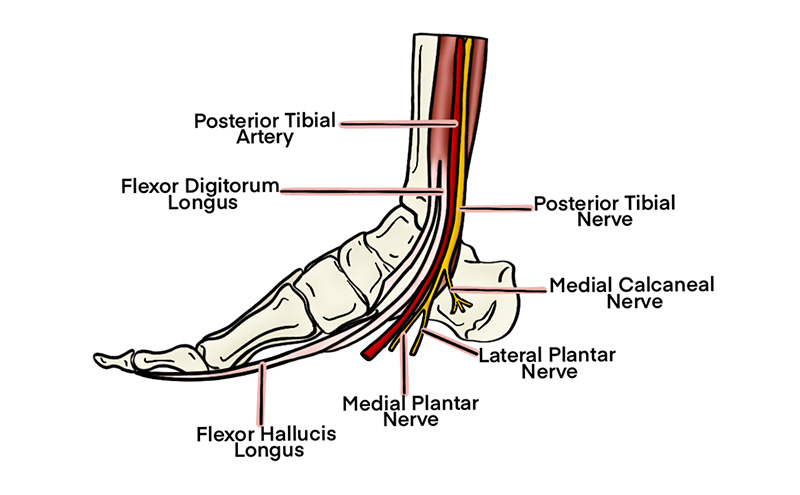
- The tibial nerve then descends through the popliteal fossa and runs deep to the soleus before emerging posterior to the medial malleolus and posterior tibial artery.
- The tibial nerve is a mixed sensory and motor nerve.
- Sensory innervation to the plantar surface of the foot
- Motor innervation to the ankle and foot flexors
Indications
- Injuries to the plantar surface of the foot
- Anesthesia prior to procedures on the plantar surface, such as laceration repair or foreign body retrieval
Contraindications
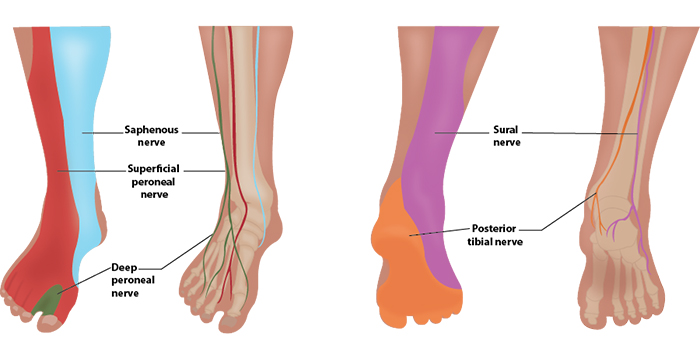
Illustration 1. Distribution of anesthesia
II. Equipment
- Probe selection: 10-15 MHz linear transducer
- Sterile transparent film dressing (e.g. Tegaderm™) or sterile probe cover
- 10ml of anesthetic of choice
- 25-30 gauge needle for skin wheal with syringe of 2-3 ml of lidocaine with epi
- 20-22 gauge needle, 1.5 inch or longer (Needle choices) depending on body habitus
III. Setup and Patient Positioning
- General procedure setup
- Patient is generally supine with the leg externally rotated and knee slightly bent.
IV. Pre-scan/Sonographic Anatomy
- A high-frequency linear array probe is applied in a transverse plane posterior to the medial malleolus.
- Probe indicator is towards the operators left.
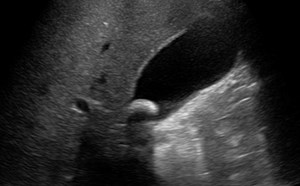
- The posterior tibial artery is the landmark structure in this area.
- The posterior tibial artery is identified by its pulsations and thick wall
- Anteromedial to the artery lies the flexor digitorum tendons and the tibialis posterior tendon (flexion of the toes will result in movement of the hyperechoic tendons in the image).
- The oval-shaped tibial nerve is found posterolateral to the posterior tibial artery.
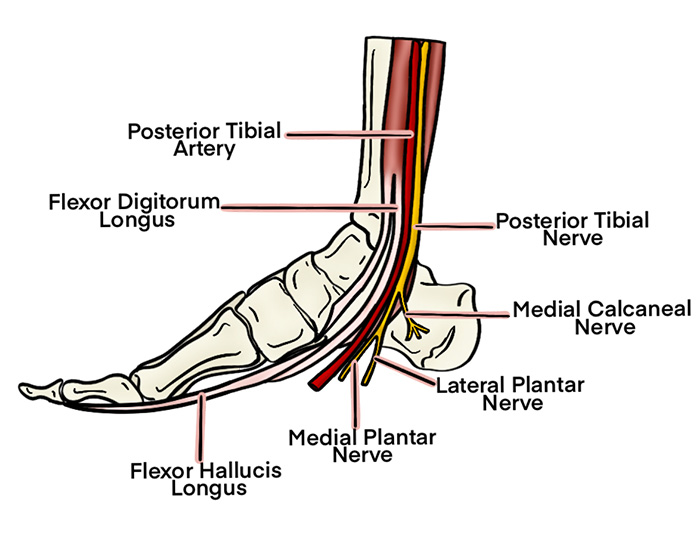
Illustration 2. Course of the tibial nerve at ankle
Video 1. Pre-scan of the tibial nerve
V. Procedure Technique
- General procedure setup
- Cover probe using sterile transparent film dressing (i.e. Tegaderm™) or sterile probe cover.
- Flush the block needle with a small amount of anesthetic to remove air
Needle Orientation
- In-plane technique is preferred but often challenging at this location due to obstructions by the achilles tendon, bony malleolus and the tibial artery.
- Tracing the nerve proximal to the malleolus may open up a needle path.
- Consider an out-of-plane technique to avoid the obstructions and place a needle directly between the nerve and artery.
In-plane Approach
- After skin anesthesia, insert the block needle 5 mm at the short side of the probe.
- Identify the needle tip by sliding the probe towards and then across the block needle (Visualizing the needle).
- Slowly advance the needle towards the deep, proximal border of the nerve.
- Once movement of the needle causes movement on the nerve (ie, ‘mechanical coupling’), inject 0.5cc of anesthetic.
- Follow injection precautions.
- If the anesthetic flows around the nerve, continue to inject in 1 cc increments until the nerve is surrounded and the block volume is reached.
- If the anesthetic is seen outside the perineural space, redirect the needle and inject another 0.5 cc.
- Readjustment of the needle position may be necessary to achieve adequate distribution of anesthesia.
- Always perform aspiration and incremental injection to avoid systemic distribution of the anesthetic.
- Typical block volumes are 5–10 cc.
- Full block onset may take up to 15–20 minutes, particularly if a long-acting anesthetic was used.
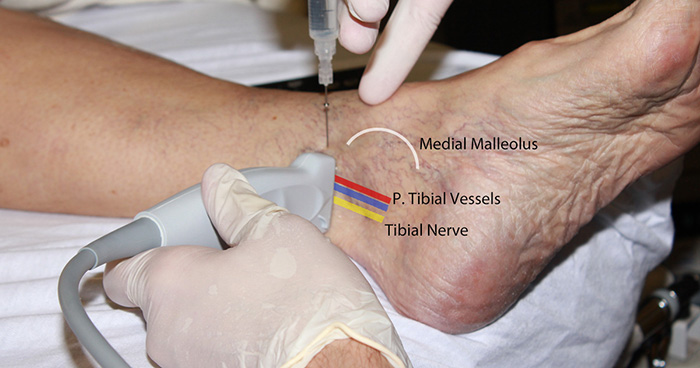
Figure 1. Tibial nerve block in-plane hands
Video 2. Tibial nerve block in-plane
Out-of-plane Approach
- The target of the out-of-plane approach is either the anterior or posterior border of the nerve. Injecting between the artery and nerve is most likely to achieve good anesthetic spread but can be challenging.
- After skin anesthesia, center the target on the image and insert the block needle 5 mm at a 45-degree angle from the center of the long side of the probe.
- Slide the probe toward the needle until the tip is seen (Visualizing the needle).
- Once the needle tip is seen, move the probe and needle in a stepwise fashion, outlined in the out-of-plane section, down toward the target
- Once the needle tip is adjacent to the artery, inject 0.5 cc of anesthetic.
- Follow injection precautions.
- If the anesthetic flows around the nerve, continue to inject in 1 cc increments until the nerve is surrounded and the block volume is reached.
- If the anesthetic is seen outside the perineural space, redirect the needle and inject another 0.5 cc.
- Readjustment of the needle position may be necessary to achieve adequate distribution of anesthesia.
- Always perform aspiration and incremental injection to avoid systemic distribution of the anesthetic.
- Typical block volumes are 5-10 cc.
- Full block onset may take up to 15–20 minutes, particularly if a long-acting anesthetic was used.
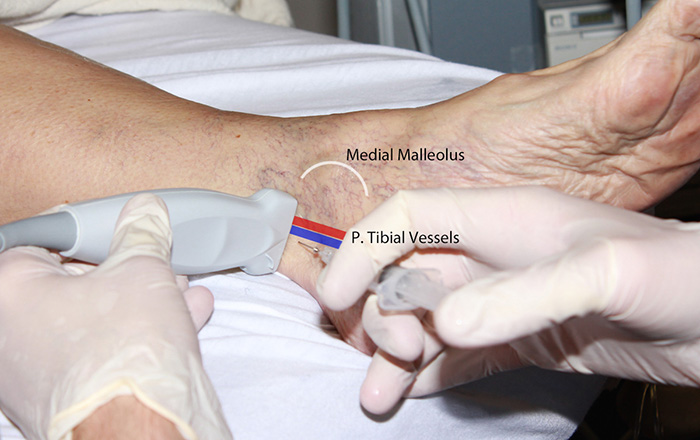
Figure 2. Tibial nerve block out-of-plane hands
Video 3. Tibial nerve block out-of-plane
VI. Post-procedure Care
- None required
- Consider marking on skin with skin pen the time and date of block performed.
VII. Pearls and Pitfalls
- If anesthetic isn’t flowing properly into the perineural space, consider using hydrodissection. With this technique, the needle is purposely advanced deeper than the nerve and then withdrawn slowly while anesthetic is injected. The anesthetic will spread the various planes apart and hopefully highlight the correct space.
- Ensure spread of local anesthetic between the artery and nerve. The out-of-plane approach can be easiest if they are closely associated.
- Placing a rolled towel or pillow underneath the calf may aid in positioning for the procedure.
- Smaller needles are more difficult to visualize using ultrasound. Novices should consider using 22-gauge needles to start.
- Avoid vascular injection and injury by frequently aspirating. Any injected anesthetic should result in a bolus of fluid on the image. If no bolus is seen after injection, this may indicate intravascular injection.
- For patients with little subcutaneous tissue, the probe may not sit well near the medial malleolus. It is sometimes necessary to perform the procedure more proximal to avoid bony projections.
VIII. References
- Redborg KE. Ultrasound improves the success rate of a tibial nerve block at the ankle. Reg Anesth Pain Med. 2009;34(3):256-60.