Deep Peroneal Nerve Block
Leonard V. Bunting, MD, FACEP
I. Overview and Indications
- The deep peroneal nerve provides sensory innervation to the skin of the first interdigital space and motor innervation to the anterior muscles of the leg and dorsum of the foot.
- Given its limited distribution it is rarely blocked in isolation.
- With planning both the deep and superficial peroneal nerves can be blocked at the ankle from one puncture site
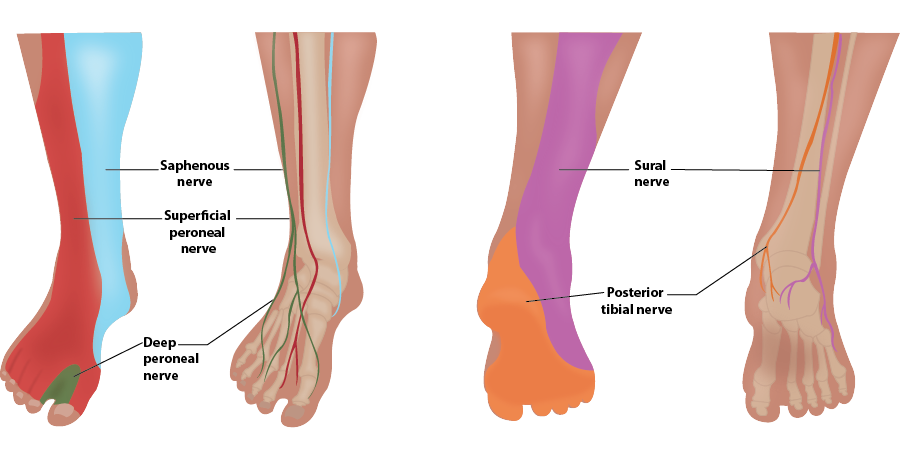
Illustration 1. Distribution of anesthesia
Indications
- Injuries to the first dorsal webspace
- Consider performing a common peroneal nerve block if a larger territory is needed
General Nerve Block Contraindications and Precautions
- Allergy to local anesthetic agents
- Active infection at the injection site
- Risk of compartment syndrome or need to monitor neurologic function
- Uncooperative patient
- Preexisting neurologic deficit that could prevent the patient from communicating paresthesia or pain during the nerve block
- Obesity obscuring nerve visualization
- Coagulopathy (relative)
II. Equipment
- Probe selection: 10-18 MHz linear transducer
- Sterile transparent film dressing (eg, Tegaderm™) or sterile probe cover
- 5ml of local anesthetic (See here for more information on choosing an anesthetic)
- 25-30 gauge needle for skin wheal with syringe of 2-3 ml of lidocaine with epi
- 22-25 gauge needle, 1.5 inch or longer depending on body habitus (See here for more information on needle selection)
III. Setup and Patient Positioning
General Procedural Setup
- Minimize ambient light to improve image quality. Placing a spotlight on the block site and darkening the rest of the room can have a dramatic effect on image quality.
- Place machine in direct field of vision of the practitioner. Avoid placement that requires twisting or head turning.
- For large volume blocks place the patient on a cardiac monitor, establish IV access and have emergency airway equipment available.
- Provide analgesics and light sedation as needed.
- Obtain consent and document a pre-block neurologic exam.
Multiple positions can be used to expose the anterior ankle. The superficial peroneal nerve can often be blocked from the same needle puncture if introduced from the medial side of the probe.
IV. Pre-scan/Sonographic Anatomy
- Anatomy
- The common peroneal nerve branches off the sciatic nerve above the popliteal fossa and courses laterally to the fibular head.
- At the upper fibula, the common peroneal nerve divides into the deep peroneal and superficial peroneal nerves.
- The deep peroneal nerve then moves anterior to run superficial to the interosseous membrane.
- At just proximal to the ankle, the deep peroneal nerve usually lies laterally to the anterior tibial artery.
- A high-frequency linear array probe is applied in a transverse plane over the anterior ankle immediately above the malleoli.
- Probe indicator is towards the operator's left.
- The anterior tibial artery is the landmark structure for this block.
- Artery is seen deep to the extensor hallucis longus and the anterior tibial tendon.
- At this level the deep peroneal nerve is commonly lateral to the artery but can be anterior or medial.
- If the nerve is not seen, quickly sliding the probe along the course of the artery may highlight the nerve.
- If the nerve is still not seen, the target of the block is to inject around the artery.
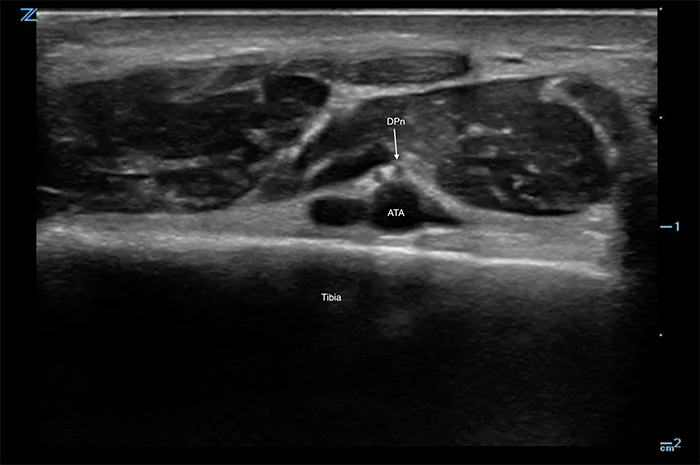
Figure 1. Deep peroneal nerve with anterior tibial artery
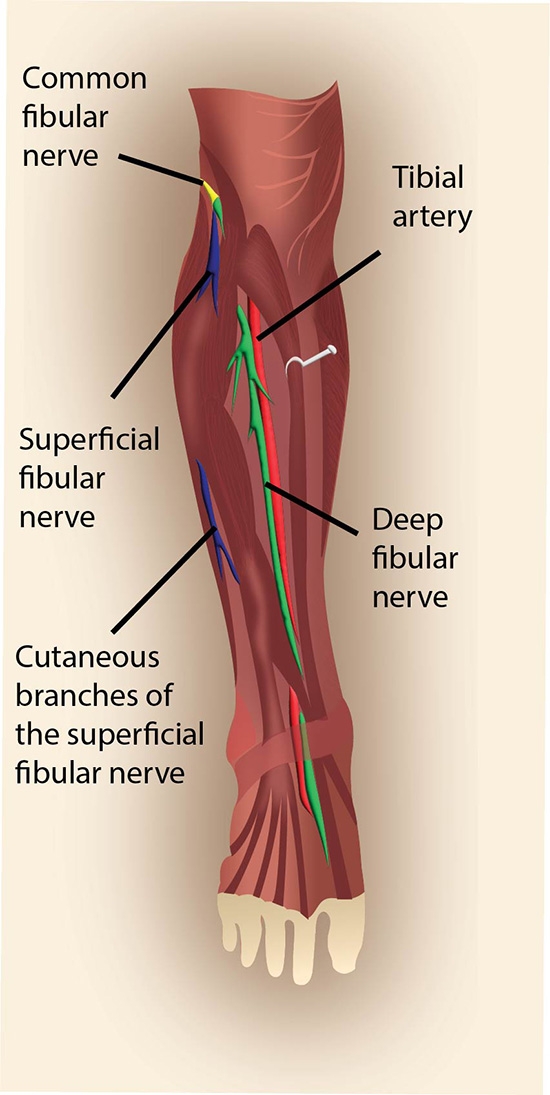
Illustration 2. Part I Deep peroneal nerve with anterior tibial artery
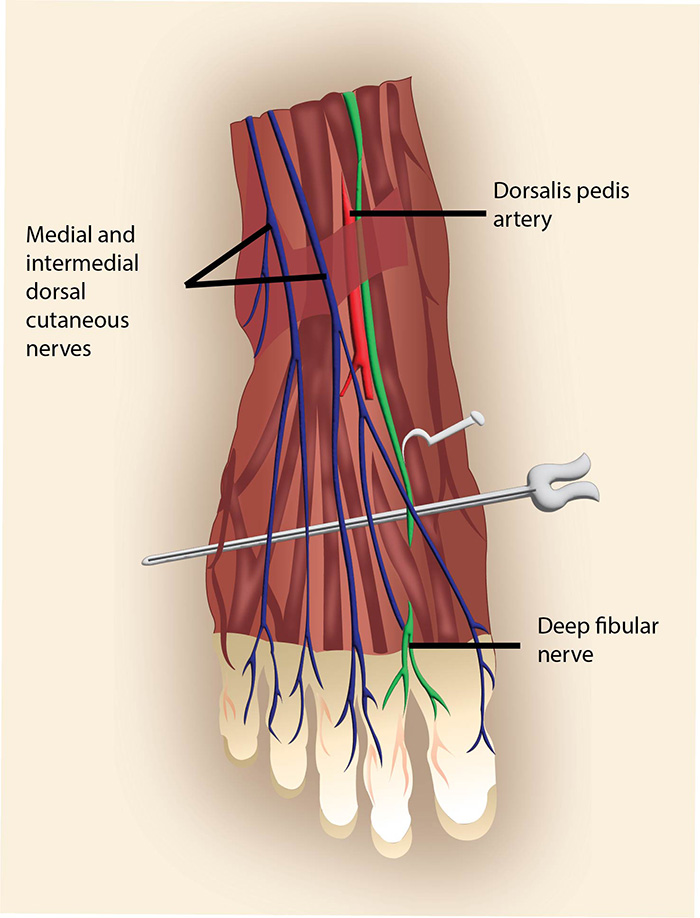
Illustration 2. Part II Deep peroneal nerve with anterior tibial artery
Video 1. Pre-scan of the deep peroneal nerve
V. Procedure Technique
- Cover probe using sterile transparent film dressing (eg, Tegaderm™) or sterile probe cover.
- Flush block needle with a small amount of anesthetic to remove air.
- An in-plane approach is preferred (See here for in-plane vs out-of-plane approach)
- After skin anesthesia, insert the block needle 3 mm at the short side of the probe.
- Identify the needle tip by sliding the probe towards and then across the block needle.
- Slowly advance the needle towards the deep, proximal border of the nerve. If the nerve is unclear, use the dorsalis pedis artery as the target.
- Once movement of the needle causes movement on the nerve (i.e. “mechanical coupling”), inject 0.5 cc of anesthetic.
- Follow general injection precautions.
- If the anesthetic flows around the nerve, continue to inject in 1 cc increments until the nerve is surrounded and the block volume is reached.
- If the anesthetic is seen outside the perineural space, redirect the needle and inject another 0.5 cc.
- Readjustment of the needle position may be necessary to achieve adequate distribution of anesthesia.
- Always perform aspiration and incremental injection to avoid systemic distribution of the anesthetic.
- Typical block volumes are 3–5 cc.
- Full block onset may take up to 15–20 minutes, particularly if a long-acting anesthetic was used.
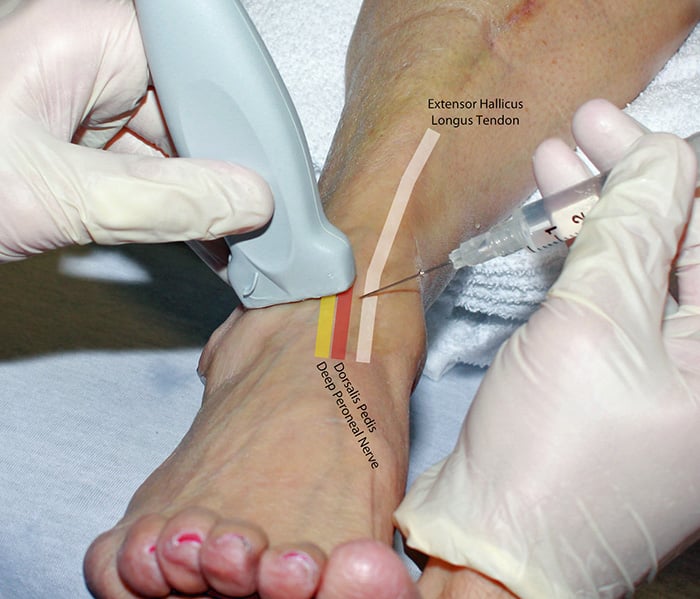
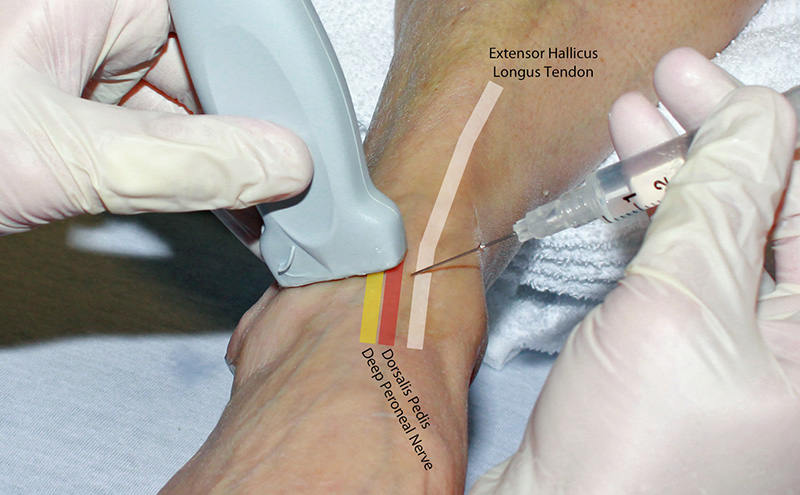
Figure 2. Hand position deep peroneal nerve block in-plane
Video 2. Deep peroneal nerve block in-plane
VI. Post-procedure Care
None required.
VII. Pearls and Pitfalls
- Ensure spread of local anesthetic between the artery and nerve. The out-of-plane approach can be easier to achieve this if the nerve and artery are closely associated.
- Plan ahead if also blocking the superficial peroneal nerve – both peroneal nerves can be blocked from one puncture site.
- The nerve will often become visible after injecting around the dorsalis pedis artery.
- A single 25 gauge, 1.5 inch needle can be used for both skin anesthesia and the block in most instances.
- Placing a rolled towel or pillow underneath the calf may aid in positioning for the procedure.