Femoral Nerve Block
Eric J. Kalivoda, MD
Leonard V. Bunting, MD, FACEP
I. Overview/Indications
- Pain management in the emergency department (ED) is a critical intervention to be addressed by emergency physicians. An integrated multidisciplinary, multimodal approach with intravenous opioid and/or anti-inflammatory medication in conjunction with ultrasound-guided regional anesthesia (USGRA) has been proposed as the future paradigm in ED management of acute traumatic pain.1
- The ultrasound-guided femoral nerve block (USGFNB) is one of the most frequently utilized regional anesthesia procedures performed by emergency physicians.2 USGFNB is generally well-tolerated with infrequent complications.3-5 Blockade of the femoral nerve and/or fascia iliaca compartment have been demonstrated as safe and effective strategies for pain management in the emergency department (ED).6-20
- USGFNB provides anesthesia to the anterior thigh, femur, and knee. Variations to the femoral nerve block, the 3-in-1 block and fascia iliaca compartment block, provide greater anesthesia to the thigh and can be helpful for more extensive proximal injuries. The 3-in-1 block and fascia iliaca compartment block both refer to blockade of three nerves with one injection: the lateral femoral cutaneous nerve, the femoral nerve and the obturator nerve.
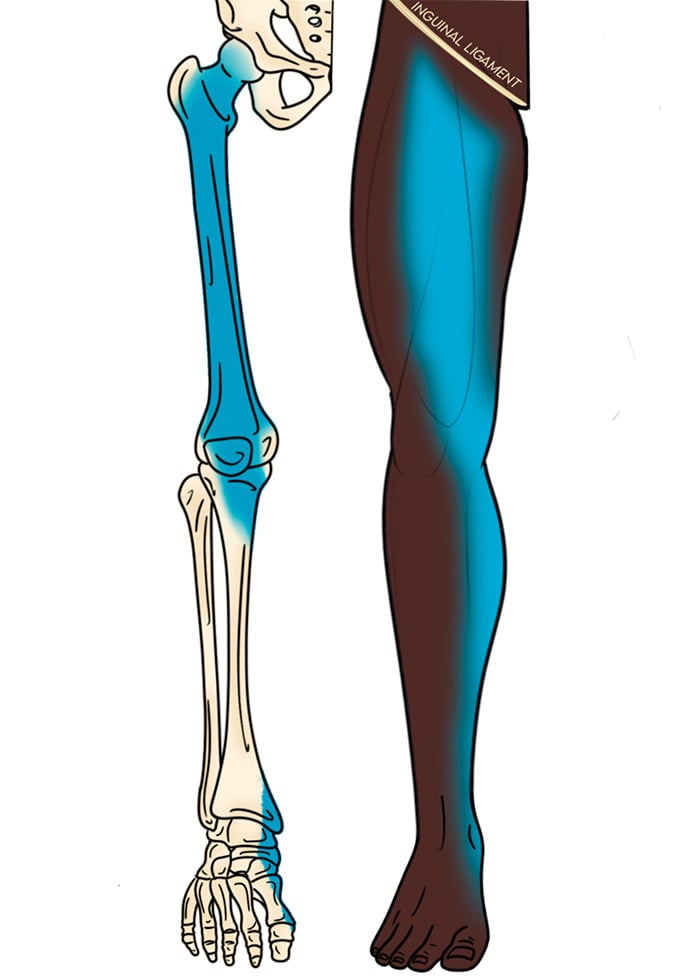
Illustration 1. Distribution of anesthesia for femoral nerve block
Indications
- Fracture or dislocation to the femur or hip
- Injury to the knee, including the patella and quadriceps tendon
- Laceration repair, burns, foreign body removal, or abscess drainage to the skin of the anterior thigh or medial lower leg
Contraindications
- General block contraindications
- Ambulatory patients as the block may impair quadriceps action for an extended period
- Isolated injuries below the knee (consider the saphenous nerve block)
II. Equipment
- Skin prep, sterile probe cover and sterile gel
- 5-12 MHz linear array probe
- 27-gauge needle and syringe of 3-5 cc of 1% lidocaine with epi for skin anesthesia
- 3.5-inch, 20-22 gauge spinal needle (Needle choices)
- 30cc syringe with anesthetic
- If the block syringe and needle are difficult to maneuver, consider using extension IV tubing or several saline locks between the syringe and needle. In this setup the operator drives the needle and instructs an assistant when to inject anesthetic.
III. Set-up and Patient Positioning
- General procedure setup
- Discuss case with orthopedic surgery if applicable.
- Premedicate the patient and place them on a cardiac monitor.
- Place the ultrasound machine on the opposite side of the bed from the block site.
- Lay the patient supine with the target leg in slight external rotation if possible.
IV. Pre-scan and Sonographic Anatomy
Anatomy
- The lumbar plexus gives rise to the femoral (L2-L4), obturator (L2-L4) and the lateral femoral cutaneous nerves (L2-L3).
- The femoral nerve enters the thigh lateral to the femoral sheath and passes under the inguinal ligament.
- Distal to the inguinal ligament, the femoral nerve is covered by 2 fascial planes.
- Fascia lata is the most superficial and covers both the femoral nerve and vessels.
- Fascia iliaca is just deep to the fascia lata and covers the nerve alone, separating it from the femoral vessels.
- Along its course the femoral nerve splits into the anterior branch, which provides sensory innervation of the skin to the anteromedial thigh, and the posterior branch, which supplies the quadriceps muscle, medial knee and sensory innervation of the skin to the medial calf. Because of this, the femoral nerve block must be performed near the inguinal ligament to not miss one of its branches.
- Sensation of the medial and lateral thigh are supplied by the obturator and lateral femoral cutaneous nerves, respectively.
- With a high frequency linear array probe obtain a transverse view of the groin just inferior to the inguinal ligament with the probe indicator to the operator’s left.
- Depth is initially set between 4 and 6 cm and adjusted as needed.
- Slide the transducer medial to lateral to visualize the femoral vessels and then center the image on the femoral artery.
- The femoral nerve lies lateral to the artery but is often not clearly visualized. Instead a triangle (see figure 1 and video 1) created by the femoral artery medially, fascia lata and iliaca anteriorly and the iliopsoas muscle posteriorly is used as the target.
Video 1. Pre-scan of the femoral region
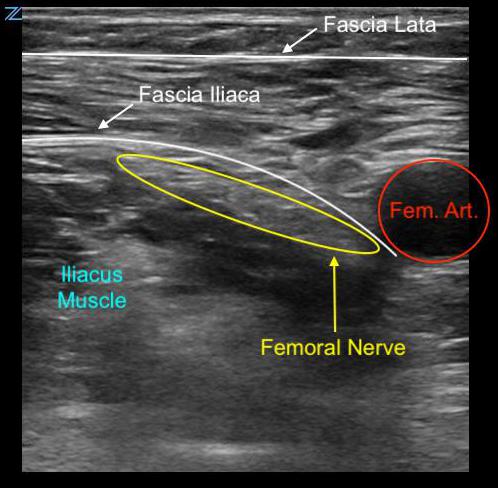
Figure 1. Transverse anatomy of the femoral triangle
V. Technique
- Prepare the site and probe in a sterile fashion.
- Probe indicator oriented to operator’s left.
- The target of the block is to inject local anesthetic around the femoral nerve. If it is not well visualized, which is common, aim to inject at the apex of the triangle lateral to the femoral artery described above in the pre-scan section.
- In-plane approach is preferred from the lateral side of the probe.
- Create a skin wheal at the target needle entry site.
- Insert the block needle ~0.5-1 cm from the lateral border of the transducer at a 30-degree angle.
- Ensure the needle is always in view.
- Slowly advance the needle towards the target – pops may be felt in the needle as the fascia lata and iliaca are punctured.
- Once movement of the needle causes movement in the target, inject a small bolus (~1 mL) of local anesthetic. The test bolus will appear as anechoic fluid seeming to flow medially and separate the elements of the tissue lateral to the femoral artery. If the bolus is not seen, stop further injections and reposition the needle. Often the initial injection is too superficial, and the needle needs to be advanced.
- Follow injection precautions.
- Once the needle is appropriately placed, inject several more ~1-5 mL aliquots until a total of 15 – 20 mL of local anesthetic is administered. Anechoic fluid should ideally encircle all borders of the femoral nerve but is not absolutely necessary to ensure a successful blockade.
- Repositioning of the needle may be required to achieve anesthetic infiltration at the anterior and medial borders of the nerve.
- Always perform aspiration and incremental injection to avoid systemic distribution of the anesthetic.
- Full block onset may take up to 15-20 minutes, particularly if a long-acting anesthetic was used.
- 3-in-1/Fascia Iliaca Compartment Block technique:
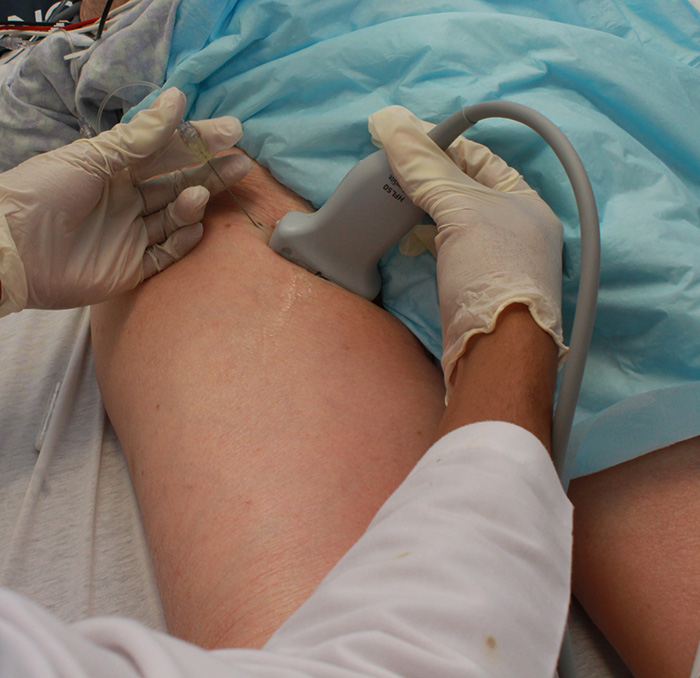
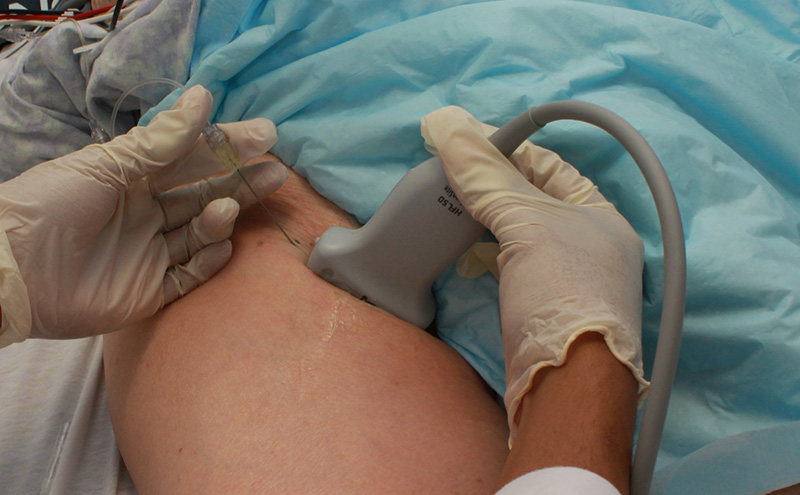
Figure 2. Hand positioning for the femoral block
Video 2. Femoral nerve block
- These blocks have an expanded distribution on the thigh (see Illustration 2).
- The technique for these blocks is similar to the USGFNB with 3 differences:
- A larger volume of local anesthetic is used to aid spread. A minimum volume of 20 mL is recommended but up to 30 –60 mL may be required. If the total dose is approaching the toxic limit, dilute it in saline to achieve a larger volume. For example, the provider can dilute 15 mL of local anesthetic (bupivacaine 0.5% or ropivacaine 0.5%) into 15 mL of 0.9% normal saline.
- The second difference is that during injection of the local anesthetic, pressure is applied 2-4 cm distal to the needle site and held for 30 seconds by an assistant. This encourages spread of anesthetic agent.
- Unlike the femoral nerve block, the needle tip does not need to be close in proximity to the nerve. Instead, insert needle and deposit anesthetic deep to the fascia iliaca (and over iliacus muscle) at a distance of approximately 1-2 cm lateral to the femoral nerve to bathe the compartment.
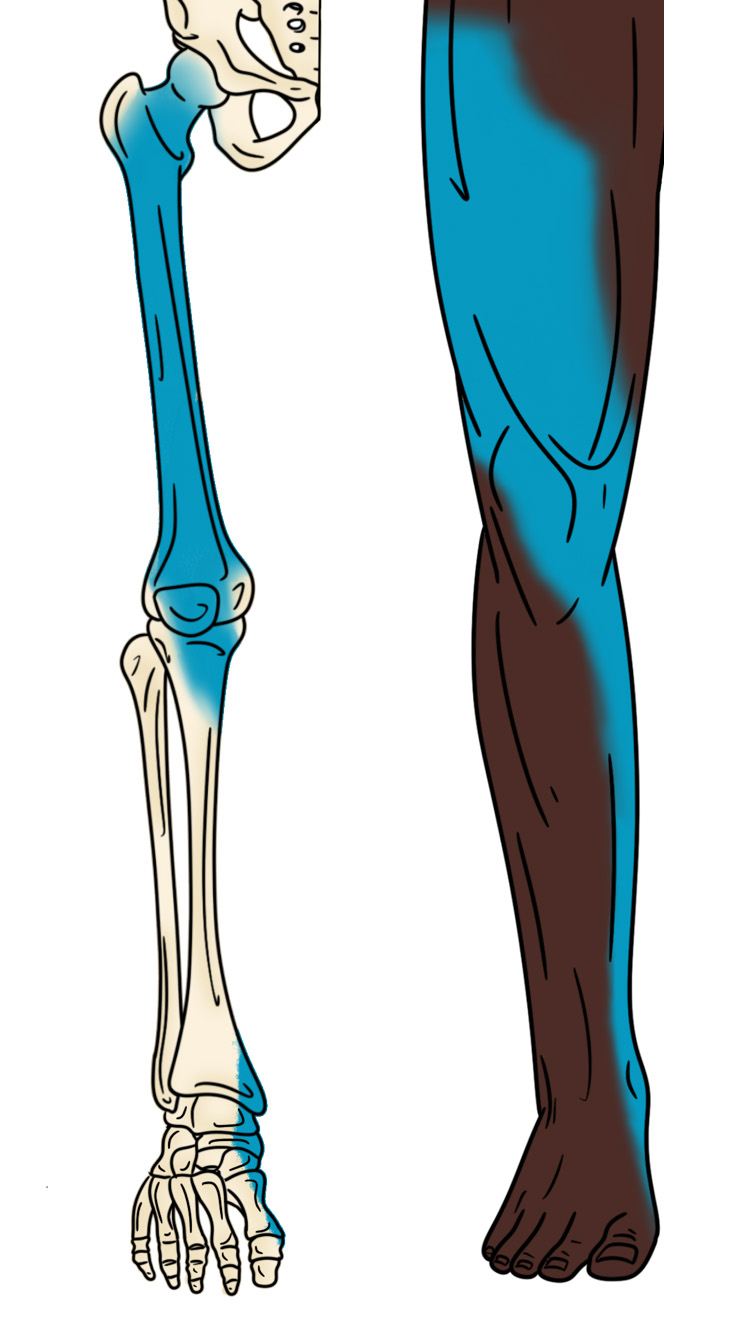
Illustration 2. Distribution of anesthesia for fascia iliaca block
Video 3. Fascia iliaca block
VI. Post-procedure Care
- Complete the appropriate procedural documentation.
- Follow-up with the patient to assess for a successful reduction in pain, as paresthesia should occur within 15 – 30 minutes of the procedure.
VII. Pearls and Pitfalls
- The needle angle should be as shallow as possible as it greatly improves needle visualization. The entire needle and tip should be well visualized during the entirety of the procedure.
- All nerves have an inherent ultrasound characteristic called anisotropy, which is an artifact that causes the echogenicity of a structure to change as the angle of insonation is changed. Whenever imaging nerves, fan the probe until they are bright and clear on the ultrasound screen.
- Local anesthetic must separate the femoral nerve from the lateral border of the femoral artery. If the nerve fails to dissect away from the femoral artery, consider an out-of-plane approach to position the needle and anesthetic bolus between the two structures.
VIII. References
- Johnson B, Herring A, Shah S, et al. Door-to-block time: prioritizing acute pain management of femoral fractures in the ED. Am J Emerg Med. 2014;32(7):801-3.
- Amini R, Kartchner JZ, Nagdev A, et al. Ultrasound-guided nerve blocks in emergency medicine practice. J Ultrasound Med. 2016;35(4):731-6.
- Marhofer P, Schrogendorfer K, Koinig H, et al. Ultrasonographic guidance improves sensory block and onset time of three-in-one blocks. Anesth Analg. 1997;85(4):854-7.
- Casati A, Baciarello M, Di Cianni S, et al. Effects of ultrasound guidance on the minimum effective anaesthetic volume required to block the femoral nerve. Br J 2007;98(6):823-7.
- Oberndorfer U, Marhofer P, Bosenberg A, et al. Ultrasonographic guidance for sciatic and femoral nerve blocks in children. Br J Anaesth. 2007;98(6):797-801.
- Van Leeuwen FL, Bronselaer K, Gilles M, et al. The ‘three in one’ block as locoregional analgesia in an emergency department. Eur J Emerg Med. 2000;7(1):35-8.
- Fletcher AK, Rigby AS, Heyes FLP. Three-in-one femoral nerve block as analgesia for fractured neck of femur in the emergency department: a randomized, controlled trial. Ann Emerg Med. 2003;41(2):227-33.
- Mutty CE, Jensen EJ, Manka MA, et al. Femoral nerve block for diaphyseal and distal femur fractures in the emergency department. J Bone Joint Surg Am. 2007;89(12):2599-603.
- Reid N, Stella J, Ryan M, et al. Use of ultrasound to facilitate accurate femoral nerve block in the emergency department. Emerg Med Australas. 2009;21(2):124-30.
- Beaudoin FL, Nagdev A, Merchant RC, et al. Ultrasound-guided femoral nerve blocks in elderly patients with hip fractures. Am J Emerg Med. 2010;28(1):76-81.
- Christos SC, Chiampas G, Offman R, et al. Ultrasound-guided three-in-one nerve block for femur fractures. West J Emerg Med. 2010;11(4):310-3.
- Elkhodair S, Mortazavi J, Chester A, et al. Single fascia iliaca compartment block for pain relief in patients with fractured neck of femur in the emergency department: a pilot study. Eur J Emerg Med. 2011;18(6):340-3.
- Haines L, Dickman E, Ayvazyan S, et al. Ultrasound-guided fascia iliaca compartment block for hip fractures in the emergency department. J Emerg Med. 2012;43(4):692-7.
- Beaudoin FL, Haran JP, Liebmann O. A comparison of ultrasound-guided three-in-one femoral nerve block versus parenteral opioids alone for analgesia in elderly emergency department patients with hip fractures: a randomized controlled trial. Acad Emerg Med. 2013;20(6):584-91.
- Groot L, Dijksman LM, Simons MP, et al. Single fascia iliaca compartment block is safe and effective for emergency pain relief in hip-fracture patients. West J Emerg Med. 2015;16(7):1188-93.
- Reavley P, Montgomery AA, Smith JE, et al. Randomized trial of the fascia iliaca block versus the ‘3-in-1’ block for femoral neck fractures in the emergency department. Emerg Med J. 2015;32(9):685-9.
- Dickman E, Pushkar I, Likourezos A, et al. Ultrasound-guided nerve blocks for intracapsular and extracapsular hip fractures. Am J Emerg Med. 2016;34(3):586-9.
- Morrison RS, Dickman E, Hwang U, et al. Regional nerve blocks improve pain and functional outcomes in hip fracture: a randomized controlled trial. J Am Geriatr Soc. 2016;64(12):2433-2439.
- Riddell M, Ospina M, Holroyd-Leduc JM. Use of femoral nerve blocks to manage hip fracture pain among older adults in the emergency department: a systematic review. CJEM. 2016;18(4):245-52.
- Ritcey B, Pageau P, Woo MY, et al. Regional nerve blocks for hip and femoral neck fractures in the emergency department: a systematic review. 2016;18(1):37-47.