Interscalene Nerve Block
Leonard V. Bunting, MD, FACEP
I. Introduction and Indications
- The brachial plexus is a neural bundle that provides sensory and motor innervation to the upper extremity.
- Nerve roots of C5-T1 undergo complex rearrangement before forming the terminal nerves of the upper extremity. (Illustration 3)
- The plexus can be blocked at several locations (interscalene, supraclavicular and infraclavicular).
- The more proximal the block, the more likely it is to include the shoulder and phrenic nerve and to spare the inferior trunk.
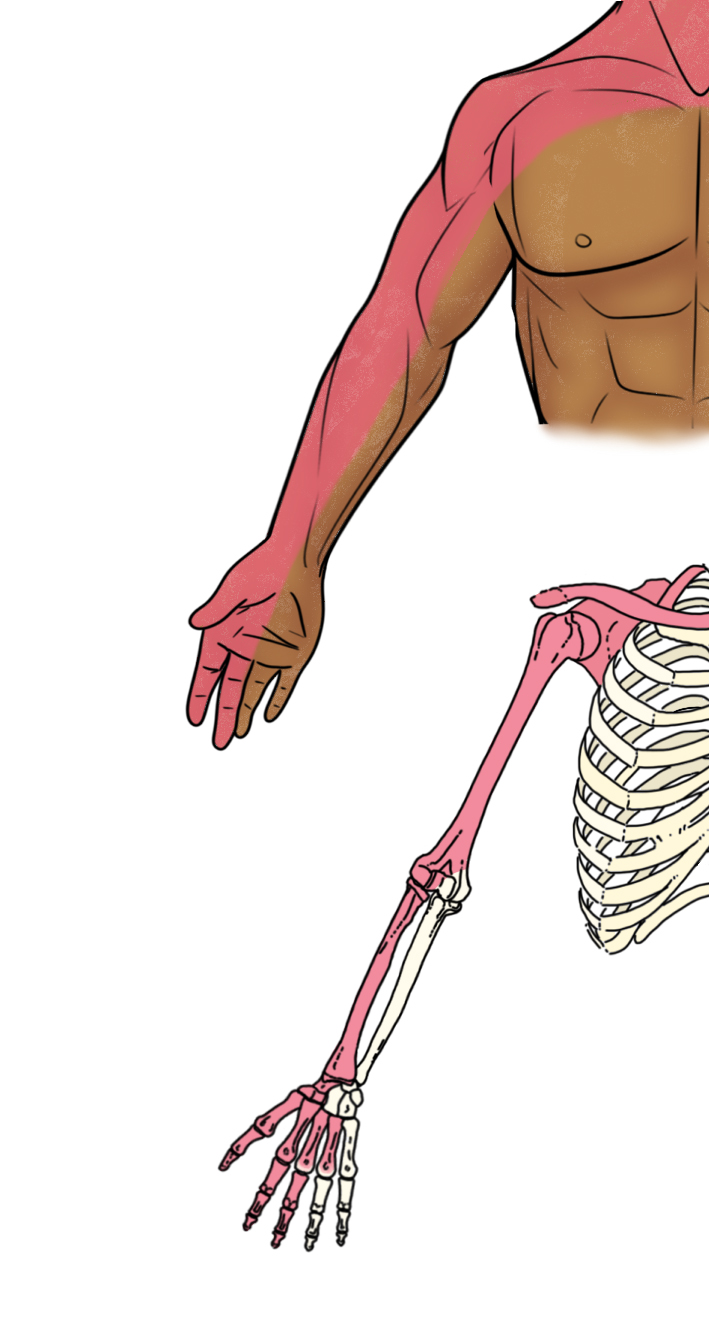
Illustration 1. Anterior distribution of interscalene nerve block
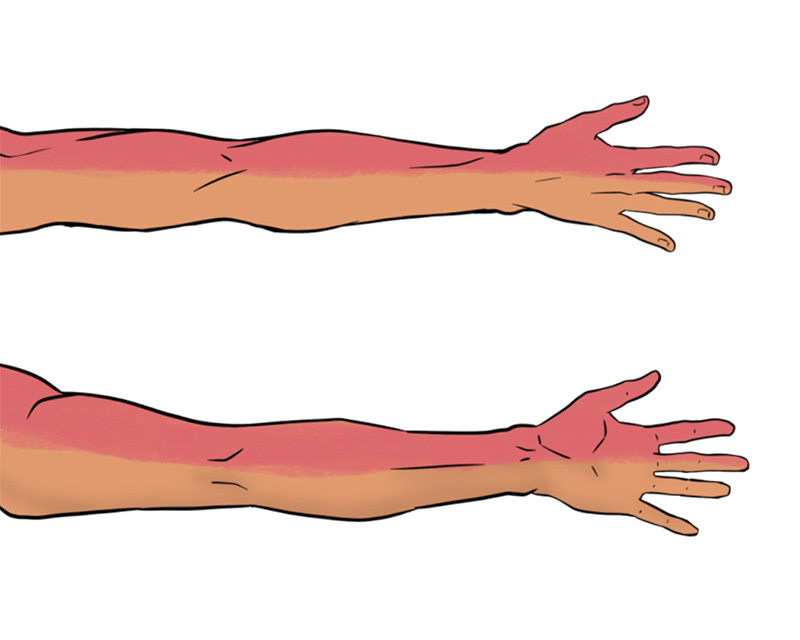
Illustration 2. Posterior distribution of interscalene nerve block
Indications
- Injury to the shoulder (dislocation, abscess, burn, fracture) or upper arm (fracture, burn, infection)
- Anesthesia for shoulder/elbow reduction or humerus fracture manipulation
Contraindications
- General block contraindications
- Lung disease or debility (causes ipsilateral diaphragm paralysis)
- Injuries below the elbow
II. Equipment
- Skin prep and sterile probe cover
- 8-12 MHz linear array probe
- 27-gauge needle and syringe of 3-5 cc of 1% lidocaine with epi for skin anesthesia
- 1.5 to 3.5 inch, 22-gauge spinal needle (Needle choices)
- 30cc syringe with anesthetic
III. Setup and Patient Positioning
- General procedure setup
- Ultrasound machine is usually placed on the opposite side of the bed from the block site.
- Patient is positioned supine or semi-recumbent with their head rotated 45 degrees to the contralateral side.
- If the stretcher prevents free movement of the block needle, place a pillow or large towel roll behind the ipsilateral shoulder or shift the patient closer to the ipsilateral side of the mattress to create free space behind the block site.
IV. Pre-scan and Sonographic Anatomy
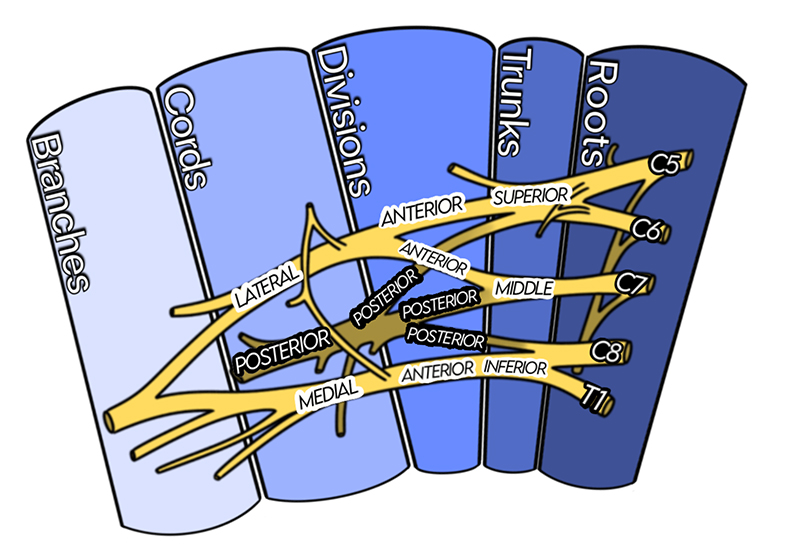
Illustration 3a. Course of the Brachial Plexus
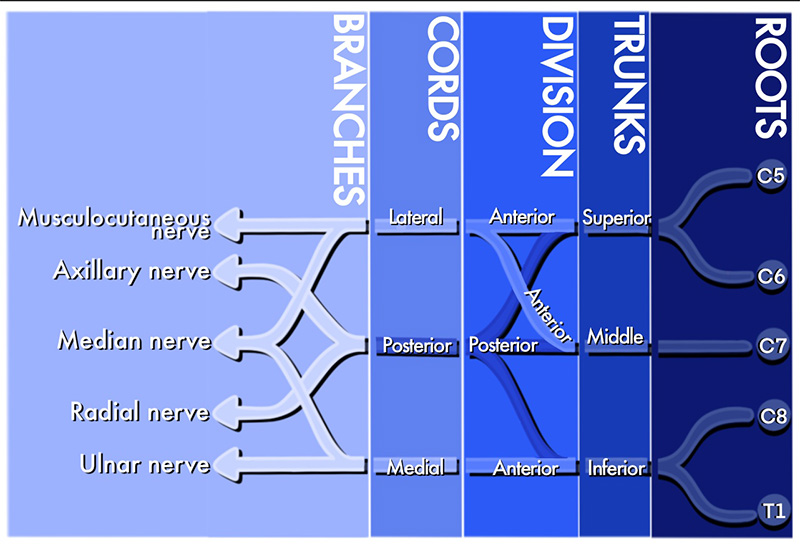
Illustration 3b. Course of the Brachial Plexus
Video 1. Interscalene pre-scan
- Interscalene Space Anatomy
- The interscalene space is a potential space between the anterior and middle scalene muscles in the neck at approximately the height of C6 transverse process and cricoid cartilage.
- The C5-T1 roots form a vertical bundle in this space consisting of superior, middle and inferior trunks.
- The trunks course inferolateral from the interscalene space to join the subclavian artery in the supraclavicular space. (Illustration 4)
- Although the region of innervation includes the entire arm, an interscalene block may spare the inferior trunk so reliable block territory excludes this region.
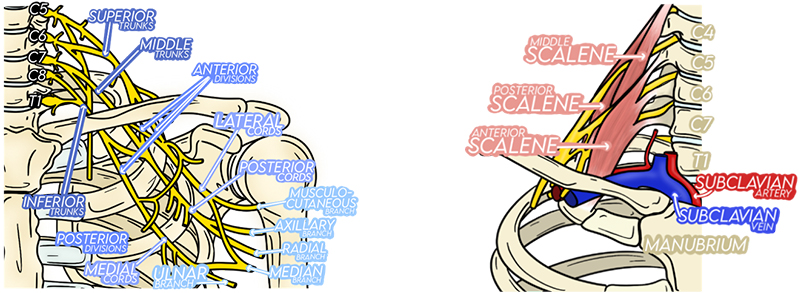
Illustration 4. Trunks associate with subclavian artery in supraclavicular space
- Pre-scan: Transverse Sweep
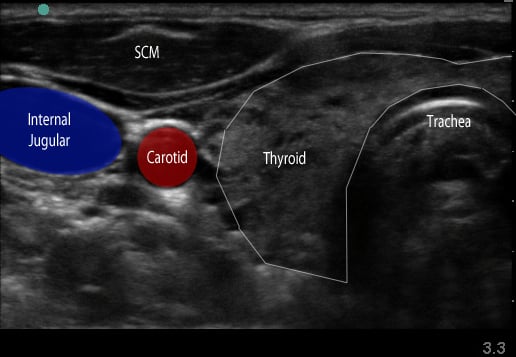
Figure 1. Transverse view over the sternocleidomastoid
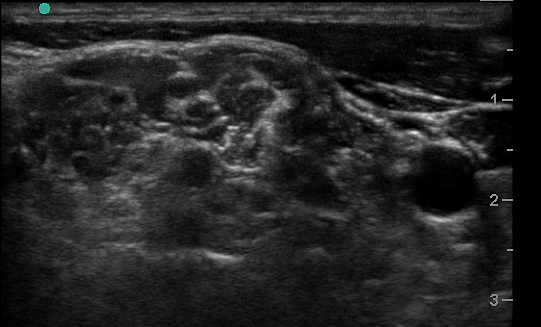
Figure 2a. Transverse view through the interscalene space
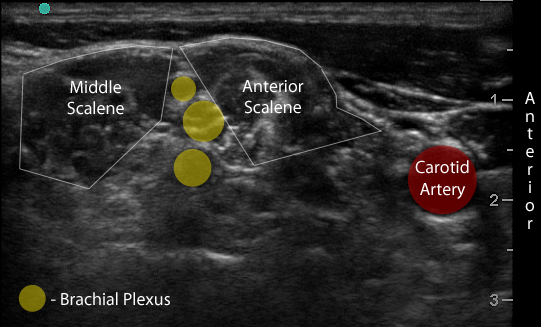
Figure 2b. With labels
-
- Use a high-frequency 8-12 MHz linear probe and begin scanning transversely over the anterior neck at the level of the cricoid. (Figure 1)
- Probe indicator oriented to operator’s left.
- Depth should be set between 4-8 cm, depending on the size of the patient’s neck.
- Trachea should be clearly seen as a midline hyperechoic arc.
- Slide the probe laterally to the lateral border of the sternocleidomastoid (SCM) (Figure 1), which is a thin muscle superficial to the carotid and jugular.
- Move the probe inferiorly to identify the anterior scalene muscle deep to the lateral border of the SCM. (Figure 2)
- Triangular muscle that is thicker caudally
- Lateral to the internal jugular vein
- If not apparent, slide the probe in a cranio-caudal direction along the lateral border of the SCM to find it
- Identify the middle scalene muscle posterior to the anterior scalene muscle.
- The interscalene space is between these 2 scalene muscles and contains the brachial plexus
- Visualize the brachial plexus here as a stack of circles with hypoechoic centers
- The plexus will look more echogenic, bundled and honeycombed in the caudal interscalene space
- Alternative Pre-scan – Backtracking from the Supraclavicular Space
Video 2. Interscalene to supraclavicular fossa
-
- Identify the brachial plexus in the supraclavicular fossa as in the supraclavicular brachial plexus block
- The subclavian artery is the main landmark at this site.
- The brachial plexus is seen immediately adjacent to the superior-posterior border of the subclavian artery as a grouping of small hyperechoic circles with hypoechoic centers, similar to a cluster of grapes.
- Backtrack from this site to the interscalene space by sliding the probe cephalad while keeping the plexus in the center of the image.
- The plexus will change conformation and become more hypoechoic as you slide superiorly.
- May take several passes up the neck and back down to the supraclavicular space.
- Moving the probe quickly may help identify the anatomy.
V. Interscalene Nerve Block Technique
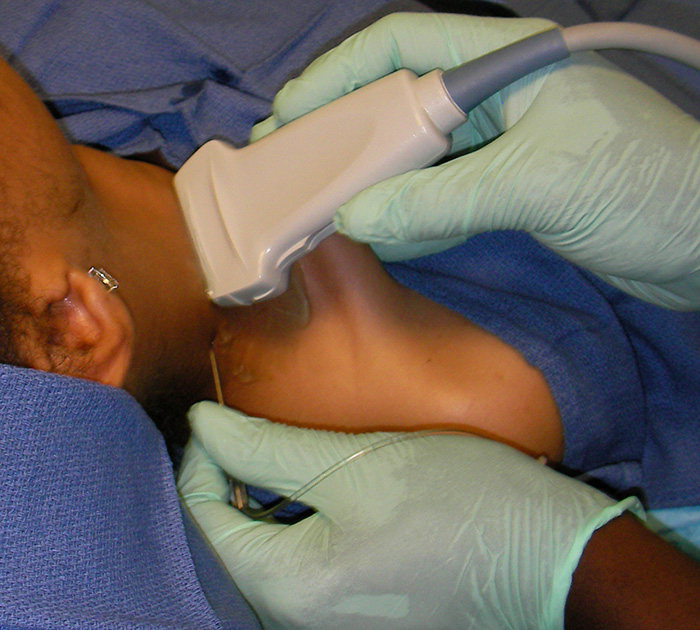
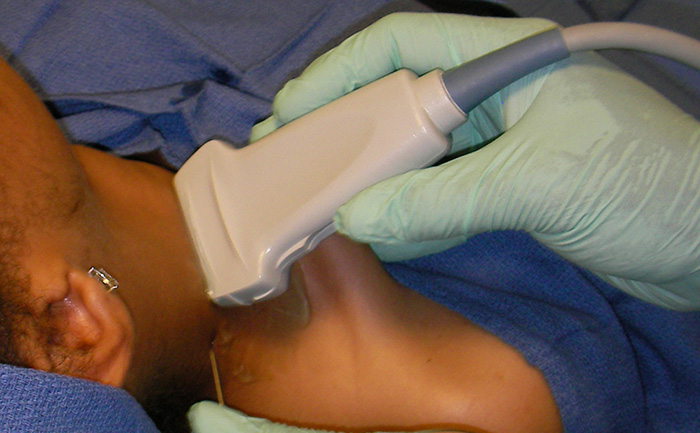
Figure 3. Needle placement for the interscalene block
Video 3. Interscalene nerve block
- In-plane approach from the posterior side of the probe is preferred.
- Probe indicator oriented to operator’s left.
- Ensure all air is ejected from skin and block needles.
- Anesthetize the block site with a skin wheal.
- Insert the block needle 5 mm at ~30 degrees to the skin surface at the posterior side of the probe.
- Identify the needle tip and ensure it is always in view.
- Advance the needle toward the plexus.
- Pass through the prevertebral fascia, which is a dense, echogenic layer overlying the scalene muscles that resists needle penetration. It may produce a “click” felt in the needle when passed through.
- Slowly advance the needle towards the plexus.
- Goal is to inject between elements of the plexus.
- Care is taken not to violate the individual elements of the plexus.
- Common target is between the top and second trunk.
- Once movement of the needle causes movement on the plexus, injection may begin.
- Follow injection precautions.
- Initially inject 0.5 cc.
- Appropriate needle placement is confirmed by movement of the plexus away from the needle and flow of the anesthetic around the entire plexus.
- If the needle is too superficial fluid will instead deposit in the scalene muscle and make it appear more echogenic.
- Readjustment of the needle may be necessary to achieve adequate distribution of anesthesia.
- Always perform aspiration and incremental injection to avoid systemic distribution of the anesthetic.
- Once appropriate needle placement is confirmed, continue to inject in 1-5 cc aliquots until the plexus is bathed in anesthetic and the total block volume is reached.
- Typical volume of local anesthetic administration is between 15 and 45 cc,1 although sufficient anesthesia has been reported with smaller volumes.2
- Digital pressure superior to the block and up to 45-degree head elevation may facilitate deep distribution of the anesthetic and blockade of the lower trunk.3
- One-time injection can provide 8–10 hours of anesthesia and up to 18 hours of analgesia when long-acting medication is used.4
VI. Pearls and Pitfalls
- The ipsilateral phrenic nerve overlies the anterior scalene muscle near the interscalene space. (Figure 4) It is affected during an interscalene nerve block,5 suspected to occur via anterior spread of the anesthetic. Although this complication is associated with a significant reduction in pulmonary function tests,5,6 it is well tolerated in most healthy patients.5,6 Care should be taken in patients with respiratory compromise or underlying lung disease.
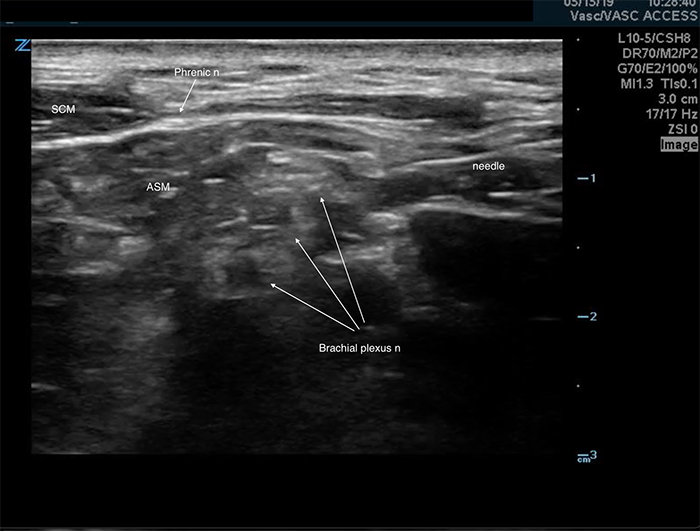
Figure 4. Phrenic nerve
- A temporary Horner’s syndrome or a hoarse voice may result from block of sympathetic afferents or the recurrent laryngeal nerve, respectively. These are self-limited and will resolve as the block wears off. However, this block is not recommended in patients with known contralateral laryngeal nerve palsy.
- It is important to avoid local anesthetic injection immediately adjacent to the transverse process and the nerve root emerging from the neural foramen because of the risk of unintentional epidural or spinal anesthesia.
- Pneumothorax can be caused by injections close to the inferior trunk and is best avoided by needle insertion and correct angulation at the C6 level. This will keep the dome of the lung distant from the needle tip.
- Incomplete head rotation can place the SCM over the plexus and block the needle path. (Figure 5) Additional rotation will move the SCM muscle out of the path. (Figure 6)
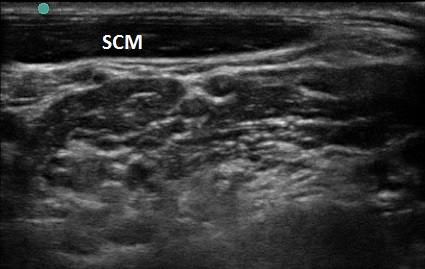
Figure 5. SCM with improper head turn
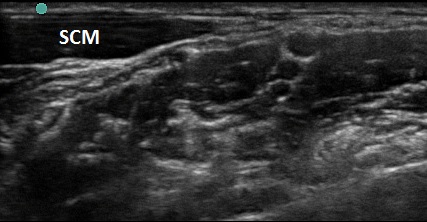
Figure 6. SCM with proper head turn
- Remember that the anterior scalene muscle can be much smaller in the more cephalad region and will increase in size when scanned more caudally.
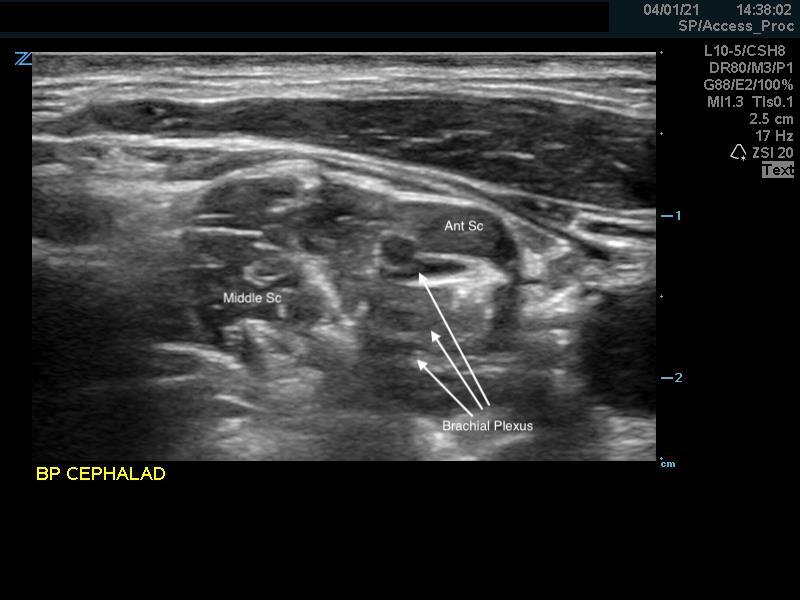
Figure 7. Anterior scalene muscle cephalad
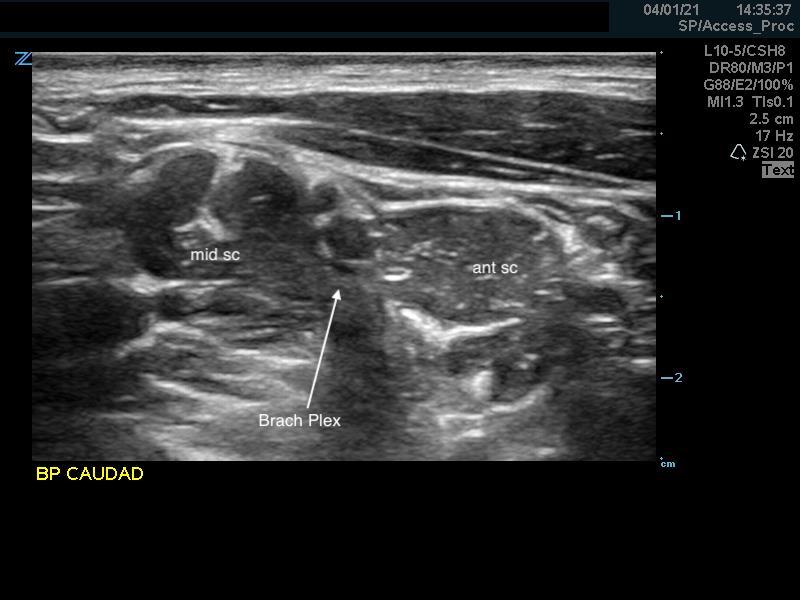
Figure 8. Anterior scalene muscle caudal
VII. References
- Borgeat A, Blumenthal S. Interscalene Brachial Plexus Block. In Hadzic A (ed). Textbook of Regional Anesthesia. McGraw-Hill, 2007, p 413.
- Riazi S, Carmichael N, Awad I, Holtby RM, McCartney CJ. Effect of local anaesthetic volume (20 vs 5 ml) on the efficacy and respiratory consequences of ultrasound-guided interscalene brachial plexus block. Br J Anaesth, 2008, 101(4):549-56.
- Borgeat A, Blumenthal S. Interscalene Brachial Plexus Block. In Hadzic A (ed): Textbook of Regional Anesthesia. McGraw-Hill, 2007, p 413.
- Borgeat A, Blumenthal S. Interscalene Brachial Plexus Block. In Hadzic A (ed):Textbook of Regional Anesthesia. McGraw-Hill, 2007, pp 414-5.
- Hortense A, Perez MV, Amaral JL, Oshiro AC, Rossetti HB. Interscalene brachial plexus block. Effects on pulmonary function. Rev Bras Anesthesiology, 2010;60:130-7.
- Casati A, Fanelli G, Aldegheri G, Berti M, Colnaghi E, Cedrati V, Torri G. Pulmonary function changes after interscalene brachial plexus anesthesia with 0.5% and 0.75% ropivacaine: a double-blinded comparison with 2% mepivacaine. Br J Anaesth.1999;83(6):872-5.