Introduction to Nerve Blocks
Leonard V. Bunting, MD, FACEP
I. Overview
Nerve blocks offer many advantages over traditional methods of anesthesia/analgesia in the ED.
- Target relief to a specific site or region
- Provide pain relief for up to 24 hours
- Little to no burden on ancillary staff or post-procedure observation
- High patient satisfaction1-3
- Decreased length of stay1
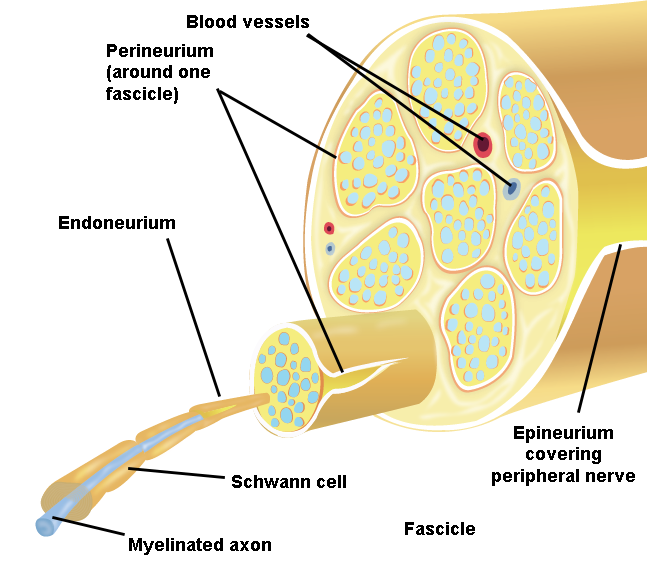
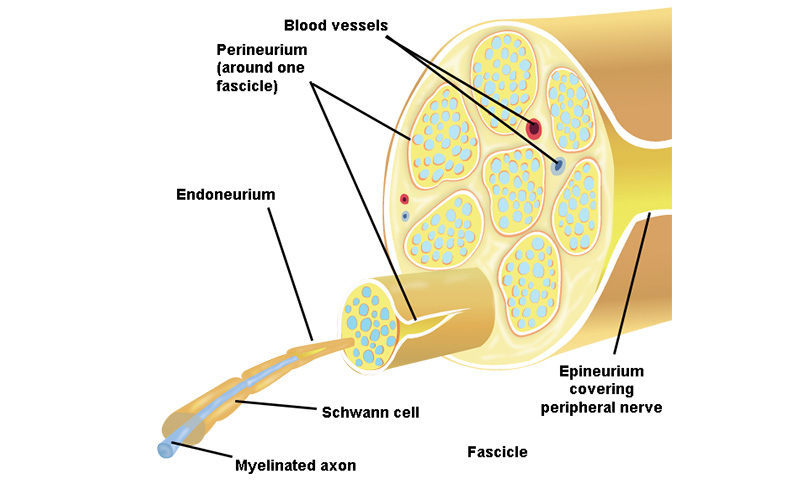
Illustration 1. Anatomy of Peripheral Nerves
Indications
- Acute regional pain management (fractures, burns, infections, chronic pain)
- Anesthesia of the extremity for a procedure (suturing, I&D, fracture/joint reduction, burn debridement)
- Alternative to procedural sedation
- Alternative to narcotics in certain patient populations (extremes of age, head injuries, altered mental status, patients on buprenorphine)
Contraindications
- Allergy to local anesthetic agents
- Active infection at injection site
- Risk of compartment syndrome or need to monitor neurologic function
- Uncooperative patient
- Pre-existing neurologic deficit that could prevent the patient from communicating paresthesia or pain during the nerve block
- Obesity obscuring optimal visualization
- Coagulopathy (relative)
II. Anatomy of Peripheral Nerves
Peripheral nerves are composed of bundles of neurons, or nerve fascicles, which are enclosed by a connective tissue called the perineurium.
- Fascicles are further bundled and held together by the loose connective tissue of the endoneurium.
- This nerve complex is enclosed within epineurium, the outermost layer of a peripheral nerve.
III. Scanning Techniques and Normal Findings
Normal Sonographic Appearance of Peripheral Nerves
- Classically, nerves have a honeycomb-like appearance in cross section caused by bundling of hypoechoic nerve fascicles within hyperechoic peri- and endoneurium.
- Distal or smaller nerves contain smaller amounts of myelinated axons and can instead look like the cut end of a rope and mimic the appearance tendons.
- Nerves may be oval, round or triangular and often change shape along their course.
- The overall conformation of a peripheral nerve depends on its course and surrounding tissue.
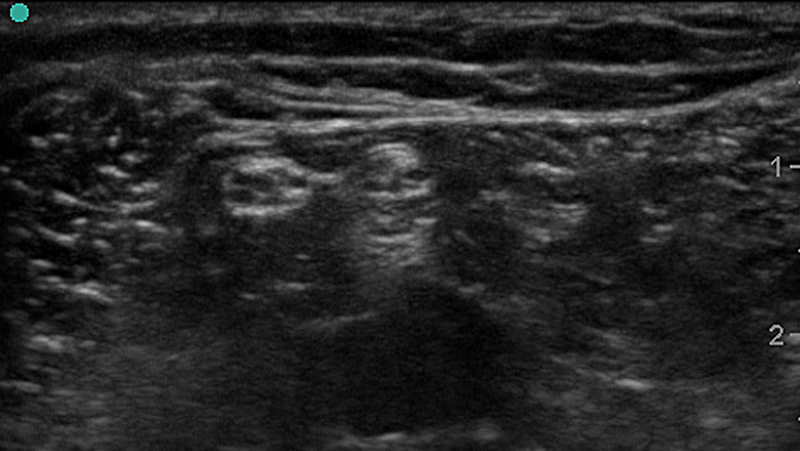
Figure 1a. Ultrasound Image of Peripheral Nerves
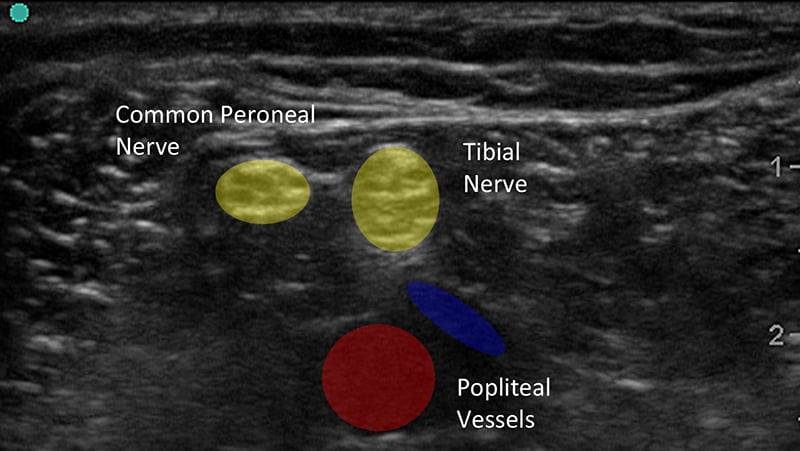
Figure 1b. Ultrasound Image of Peripheral Nerves With Labels
Identifying Nerves
- A linear array transducer is generally used to identify peripheral nerves.
- Nerves are best seen in transverse or cross-section.
- Nerves can exhibit strong anisotropy (Video 1).
- Anisotropy refers to the changes in echogenicity of a structure as the angle of insonation is changed.
- Care must be taken to adjust the angle of insonation to ensure optimal nerve visualization.
- Tendons, ligaments and muscle also exhibit anisotropy.
Video 1. Anisotropy
- Nerves can be hard to identify on ultrasound.
- Tendons, muscle and fascial planes can all look like nerves or hide them.
- Nerves are often found by their association with more easily identified structures such as blood vessels, bone or muscles.
- Multiple, rapid passes along the expected course of a nerve may highlight its location.
- Identifying a nerve distally and following it back to the site of intervention can also be helpful.
V. Pearls and Pitfalls
VI. References
- Stone MB, Wang R, Price DD. Ultrasound-guided supraclavicular brachial plexus nerve block vs procedural sedation for the treatment of upper extremity emergencies. Am J Emerg Med. 2008;26(6):706-10.
- Blaivas M, Lyon M. Ultrasound-guided interscalene block for shoulder dislocation reduction in the ED. Am J Emerg Med. 2006;24(3):293-6.
- Beaudoin FL, Nagdev A, Merchant RC, Becker BM. Ultrasound-guided femoral nerve blocks in elderly patients with hip fractures. Am J Emerg Med. 2010;28(1):76-81.
VII. Additional Reading
- Wilson JE, Pendleton JM. Oligoanalgesia in the emergency department. Am J Emerg Med. 1989;7(6):620-3.
- McQuay HJ, Carroll D, Moore RA. Postoperative orthopaedic pain – the effect of opiate premedication and local anesthetic blocks. Pain. 1988;33(3):29–5.
- Liebmann O, Price D, Mills C, Gardner R, Wang R, Wilson S, Gray A. Feasibility of forearm ultrasound-guided nerve blocks of the radial, ulnar and median nerves for hand procedures in the emergency department. Ann Emerg Med. 2006;48(5):558-62.
- Pogatzki-Zhan EM, Zahn PK. From preemptive to preventive analgesia. Current Opinion Anaesthesiol. 2006;19(5):551-5.